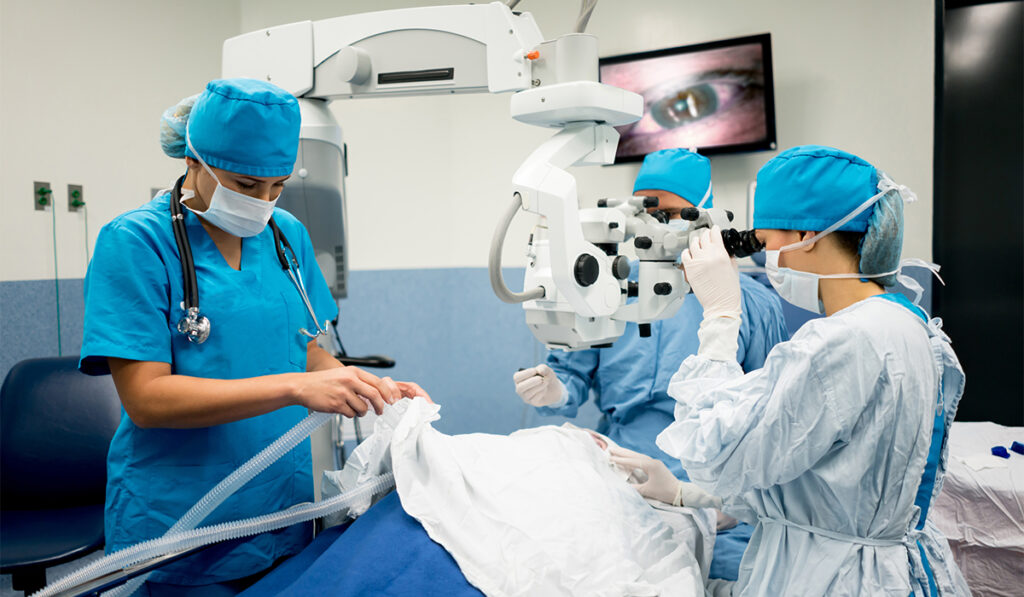
Researchers from Vanderbilt University and Vanderbilt University Medical Center have received a $1.4 million grant from the National Eye Institute at the NIH to translate technologies that enable 4D imaging of macular holes (MH) during surgical repair.
Left untreated, MH can lead to retinal detachments and vision loss. Severe cases are routinely repaired surgically; however, how much vision is restored after surgery varies from patient to patient.
“We’ll examine how different surgical techniques impact retinal health and correlate changes in retinal structure during surgery with visual outcomes after surgery,” said principal investigator Yuankai “Kenny” Tao, Ph.D., an assistant professor of biomedical engineering at Vanderbilt.
“We’ll examine how different surgical techniques impact retinal health.”
Tao will lead a team of engineers and clinicians that includes Karen Joos, M.D. and Shriji Patel, M.D., both ophthalmologists at Vanderbilt Eye Institute. The engineers and clinicians collaborate through the Vanderbilt Institute for Surgery and Engineering.
Repairing Macular Holes
Optical coherence tomography (OCT) has revolutionized ophthalmic imaging by allowing for high-resolution non-invasive visualization of retinal microstructure, and has become the gold standard for clinical diagnostics. However, despite broad adoption of preoperative OCT prior to macular hole repair, postoperative functional outcomes can be highly variable.
Standard of care for MH repair involves vitrectomy and peeling of the inner limiting membrane in the retina. Recent clinical studies have shown this surgical manipulation can lead to retinal structural changes including inner retinal dimpling, foveal shift and disruptions in photoreceptor layers.
While about 90 percent of patients achieve hole closure and anatomic normalization, as low as 27 percent achieve a best-corrected visual acuity better than 20/40.
“Differences in vision restoration after macular hole surgery are hypothesized [to be] related to the integrity of the retina during surgery; however this has not been systematically investigated,” Joos said.
Comparing Surgical Maneuvers
The researchers will use intraoperative OCT (iOCT) to perform foundational imaging studies of MH surgery to understand the effects surgical maneuvers and tractional force have on postoperative vision recovery.
“We can’t really measure force, so we’re looking at surrogate force,” Tao explained. “Essentially, we’re doing real-time quantification of deformation of tissue layers.”
To overcome the limitations of current-generation iOCT systems, Tao and his team have developed multimodal spectrally encoded coherence tomography and reflectometry (SECTR) technologies that use concurrently acquired spectrally encoded reflectance (SER) and OCT images to provide complementary spatial information and enable volumetric registration and tracking.
“We’re really excited about developing new tools to look at dynamics, which we’ve really never done before,” Tao said.
Personalizing Surgical Care
Automated tracking and 4D imaging of MH dynamics will provide unprecedented data on structural changes resulting from surgical maneuvers, which the researchers say could help predict postoperative functional outcomes. The goal is more precise surgical planning.
“The technologies … could have broad applications in personalizing surgery, predicting outcomes, and providing image-guided feedback.”
“The technologies developed during this project could have broad applications in personalizing surgery, predicting outcomes, and providing image-guided feedback in a range of surgical specialties,” Joos said.