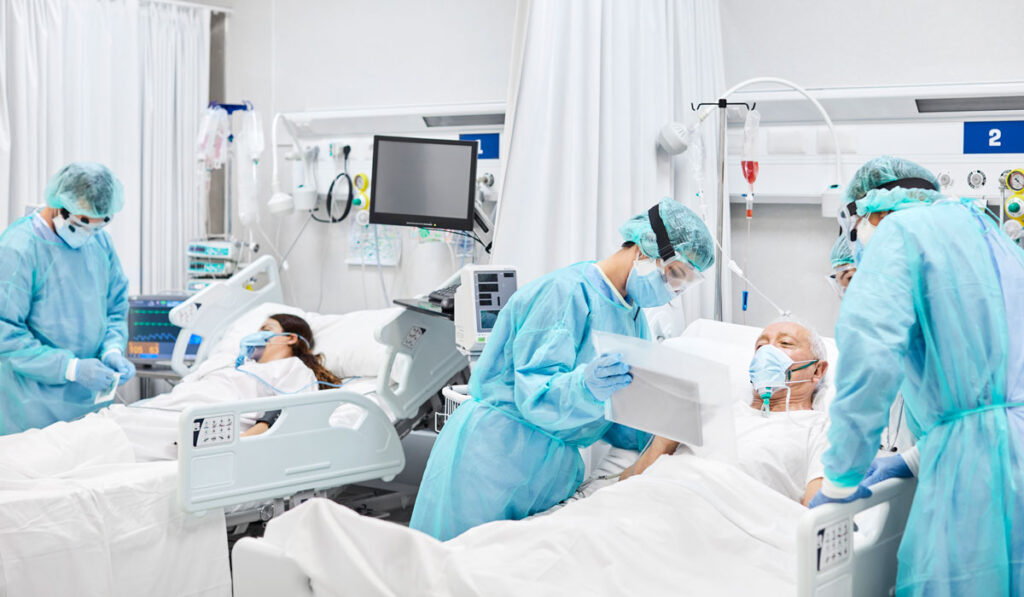
If COVID-19 had swept the globe 20 years ago, the death rate would be higher, said E. Wesley Ely, MD, MPH, co-director of the Critical Illness, Brain Dysfunction and Survivorship (CIBS) Center. The boundaries of what is survivable have expanded, but to what impact on the patient? A stay in the ICU extends well beyond the walls of a hospital and follows the patient as they try to re-enter the world.
With the volume of COVID-19 ICU survivors, the research and experience of Vanderbilt University Medical Center’s ICU Recovery Center, started in 2012, is critical to understanding the repercussions of these long ICU stays, and what people will need as they work toward recovery.
“We have to remove the depersonalization chamber and account for all the things that matter to that person. The main question I wake up wanting to answer every day is, ‘how can I help people recover fully so that their dignity is upheld so that the unique pricelessness of every human being who comes under my care, or the care of someone else in an intensive care unit is respected with the reverence that it should be — such that they feel fully human, and fully respected, and that they don’t think that they lost part of themselves in the process of critical illness,” said Ely.
‘Discharge to home is a huge drop-off’
Critical care is a relatively new specialty that exists because of the boundaries of what can be survived, have expanded with technology.
Now, it’s essential to understand and track how ICU survivors function in their daily lives. That’s a challenge for critical care physicians who often lose touch with patients after a discharge — or even a downgrade to lower levels of inpatient care.
The ICU Recovery Center, a part of CIBS, is trying to increase touchpoints and help patients navigate the obstacles – often a combination of cognitive and physical repercussions — that may have a sharp impact on their life.
“The ICU is the most intensive care you can get in the hospital … and after people leave that intensive care, they stepped down to less intensive care settings like the regular hospital ward, long-term acute care, inpatient rehab, skilled nursing facility, which is like a nursing home. And some of them go straight home,” said Carla Sevin, MD, ICU Recovery Center Director and Medical Director, Pulmonary Patient Care Center. “And that discharge to home is a huge drop-off. The system is really not geared to helping patients recover optimally from critical illness. Like I said, we suffer a little bit from an identity problem where it is not widely understood that critical illness or critical care is specialty care. There’s no defined recovery pathway. … And nobody really owns your recovery process. Nobody’s in charge of you getting all the way better.”
Predicting risk for disruption to brain activity
Physician scientists at CIBS, and colleagues around the world are finding new, better ways to protect the brain functions of people who are fighting physically to stay alive. Doctors are exploring what is happening in the brain in the ICU — whether it’s a four day or a four week stay.
“I postulate that there must be a link between the disruption in brain activity patterns acutely, and the changes in brain activity patterns that we see in the chronic long-term phase. And I’m looking to understand the link between those two. I think that’ll be useful for two reasons. One is in order to sort of help predict who’s most at risk for those long-term problems, outcomes. And also, because there may be ways to capitalize on that knowledge of the links between those brain activity patterns, to try to manipulate those patterns in the interim and rescue people from that chronic decline that we see,” said Shawniqua Williams Roberson, M.Eng., MD, assistant professor of Neurology.
Tune in on your favorite platform: Apple Podcasts, Google Podcasts, Spotify, Stitcher, Pandora, and the Health Podcast Network. New episodes drop every week.
Join the conversation on Twitter and LinkedIn with #ListenDNA and by following @VUMC_Insights.
To learn more about Vanderbilt Health DNA and access episode extras, visit www.listendna.com.