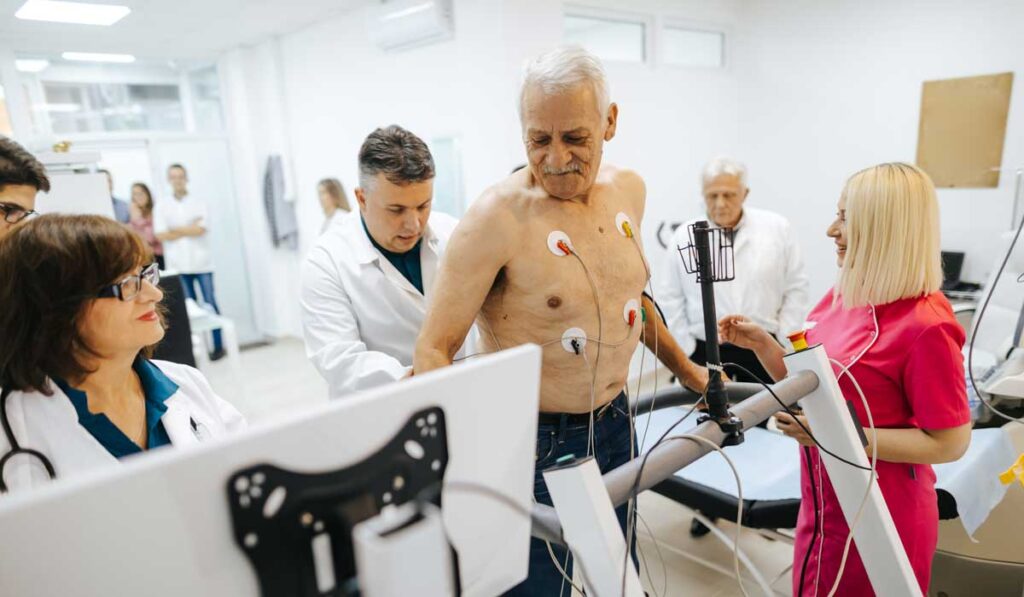
National rates of autologous and allogeneic hematopoietic stem cell transplantation (HSCT) in older adults are on the rise tracking upward with the aging population, where patient frailty is a top concern for both surviving the intense treatments and emerging with improved prospects.
“We need better evidence for how to recognize patients whose frailty can be addressed while moving toward a successful outcome, versus those unlikely to survive,” said Reena Jayani, M.D., a hematologist and stem cell transplant physician at Vanderbilt University Medical Center.
“There is data on the success of HSCT for various blood cancers in older adults, but not much work has been done to examine what happens when medicine is personalized and when frail patients undergo prehabilitation,” Jayani said.
To address this, Jayani and geriatrician Parul M. Goyal, M.D., are leading Vanderbilt’s Older Adult Stem Cell Transplant and Cellular Therapy Clinic – one of only a few centers of its kind in the nation – where they conduct comprehensive geriatric assessments and improve readiness for HSCT and chimeric antigen receptor (CAR) T cell therapy. Their focus is on identifying and tracking significant health vulnerabilities in patients 65 or older, or in younger patients who are medically frail.
The team will soon be comparing retrospective outcomes data on over 100 patients that received HSCT at Vanderbilt, with prospective data on more than 190 patients who have completed the comprehensive geriatric assessment.
“We’ve factored into the program the co-morbidities and various ways these patients may be vulnerable – including fall risk, dementia, and mental health – to help determine what personalized actions we can do around the HSCT process to weigh the risks and benefits and prepare patients for this intensive therapy,” Goyal said.
Need for Geriatric Assessment
Jayani explains that non-relapse mortality following HSCT has fallen in recent years, thanks in part to the development of lower-intensity conditioning chemotherapy regimens given during transplant, as well as newer antimicrobials, use of peripheral blood stem cells, and improved prevention and treatment for graft-versus-host disease.
While mortality and morbidity rates following HSCT rise with age, emerging data suggest that older HSCT recipients who receive comprehensive geriatric assessment with personalized interventions have significantly lower inpatient deaths, shorter length of stay in the hospital, fewer discharges to nursing homes, higher overall survival rates and lower non-relapse mortality at one year. Jayani also recently authored a literature review detailing the utility of geriatric assessment for HSCT.
A Comprehensive Evaluation
At Vanderbilt, Goyal, Jayani and colleagues assess geriatric patients on multiple predictors of poor health outcomes, including high-risk medications, cognitive impairment, declining physical function, and malnutrition.
“Our purpose here is to evaluate these risks to stratify and inform treatment plans, address deficits we identify, and then repeat the comprehensive geriatric assessment,” Goyal said. “Patients may need physical therapy before transplants to help get their physical stamina and resilience up to a better level, for example.”
The investigators also assess patients’ emotional health and may adjust their medication or provide counseling options to help them navigate stressors related to the diagnosis and intensive treatments to come.
“We’ve factored into the program the co-morbidities and various ways these patients may be vulnerable – including fall risk, dementia, and mental health – to help determine what personalized actions we can do around the HSCT process.”
Jayani notes that the measures improve overall survival rates, as well as non-relapse mortality, but also address toxicities such as arrhythmias, decreased functional status, and organ damage.
“The comprehensive geriatric assessment tool covers physical status, cognition, psychological assessment, nutritional status, polypharmacy, comorbidities, and social assessment,” Goyal said. “We incorporate this evaluation into an intensive two days of meetings with the provider team, as well as bone marrow biopsies, echocardiograms and lung-function tests. When it is completed, we come up with a plan, which is then shared with the patient and their oncologist.”
Improving Chances to Thrive
Further studies are ongoing to identify the comprehensive geriatric assessment domains or tools with the most prognostic accuracy in the HSCT setting. In the meantime, patient feedback at Vanderbilt assures Goyal and Jayani they are on the right track.
“Many patients are skeptical coming into the clinic,” Goyal said. “But they’re very happy at the end of it, because they recognize that we are talking about things that haven’t been talked about before, like being able to do those activities that enable you to live independently. We are looking at them holistically, and they appreciate that.”