The benefits of preventing breast cancer-related lymphedema have long been acknowledged, yet the importance of avoiding this potentially chronic condition is rarely stressed in clinical practice or patient education, says Cristina Kline-Quiroz, D.O., assistant professor of physical medicine and rehabilitation at Vanderbilt University Medical Center.
To address this, Kline-Quiroz is leading a lymphedema surveillance and prevention initiative that was developed to stack the odds against an unwelcome build-up of lymphatic fluids.
Supported by the Cancer Charities Settlement Fund of Rockefeller Philanthropy Advisors, the initiative identifies patients who are most at risk for chronic lymphedema. The effort uses bioimpedance measurements to identify subclinical lymphedema, opening the door to early treatment.
Working alongside Kline-Quiroz is Sheila Ridner, Ph.D., the Martha Rivers Ingram Professor of Nursing at Vanderbilt and a national leader in the research on lymphedema prevention.
“Her work is a springboard for this new program, which we rolled out this month,” Kline-Quiroz said.
“Deliberate surveillance programming is needed to measure bioimpedance before surgery and on through the pivotal months and years after surgery.”
The first fellowship-trained cancer rehabilitation physiatrist in Tennessee, Kline-Quiroz runs the program through offices in both the Vanderbilt Breast Center and Stallworth Rehabilitation Hospital. She provides care at several clinics and coordinates therapy services with providers throughout Vanderbilt’s broad catchment area to work within patients’ medical, geographical, family and job constraints.
Running Interference at the Pivot Point
Reports vary, but most specialists say lymphedema occurs in about 25 to 30 percent of patients who undergo axillary lymph node dissection. Gaining access to preventative regimens and early treatment may require patients to overcome hurdles, such as financial constraints, access of certified lymphedema therapists, encumbrances on their time, and access to transportation, Kline-Quiroz says.
“This typically requires participation in complete decongestive therapy, followed by lifelong self-care though manual lymphatic drainage, wearing compression garments, and diligent skin care and monitoring, given the increased risk of cellulitis. It can also impact the function of their arm, including their shoulder and hand.”
The onset of lymphedema can be insidious, occurring months or even years after surgery and emerging with barely perceptible symptoms. Once lymphedema develops, it often becomes a chronic condition that must be managed through daily care.
“By identifying subclinical lymphedema before changes are visible, we can initiate management and significantly reduce risks of progression to chronic and irreversible lymphedema,” Kline-Quiroz said. “This is why deliberate surveillance programming is needed to measure bioimpedance before surgery and on through the pivotal months and years after surgery.”
Bioimpedance Benefits
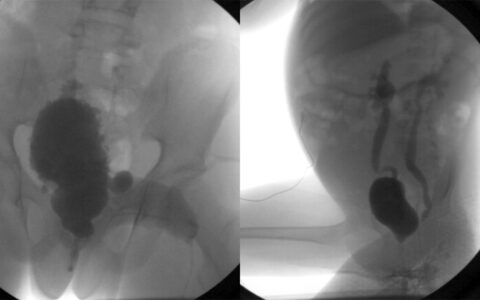
Bioimpedance spectroscopy (BIS) uses electric current to measure resistance within a breast cancer patient’s upper arm and provides information on levels of intra- and extracellular fluids, fats, and lymphatic fluid build-up.
Ridner has found BIS to be a relatively simple and low-cost way to more accurately asses lymphatic fluid build-up, as opposed to the traditional tape-measure method. Her research has demonstrated a 67 percent relative risk reduction of lymphedema when BIS is used versus the circumferential arm measurement. BIS also has clinical advantages over methods like optoelectronic perometry and dual‐energy X‐ray absorptiometry, she said.
The new initiative uses BIS to follow the recovery of breast cancer survivors under Vanderbilt’s care who are at highest risk of developing lymphedemia.
They start by taking a measurement ahead of their cancer treatment “to identify their true baseline,” Kline Quiroz said.
“We then repeat this every three months for the first three years. By catching it in the subclinical phase, we can initiate treatment, which involves wearing a compression garment every day for a month.”
Support for All Survivors
The Dayani Center for Health and Wellness at Vanderbilt offers specialized technology and lymphedema therapy for cancer survivors, meeting them wherever they area in the lymphedema spectrum.
“These specialized therapists, physical therapists and exercise physiologists individualize their care designed around the complexities of cancer, managing several novel pre-habilitation programs in addition to rehabilitation programs,” Kline-Quiroz said. “They work to help enhance patients’ ability to walk, perform activities to care for themselves, get stronger, improve range of motion, decrease swelling related to lymphedema and decrease pain.”
Just a year into her tenure at Vanderbilt, Kline-Quiroz has yet more irons in the fire. She is at the hub of programming for survivors of all cancers, who have – or are at-risk for – physical and functional impairments from treatment or from the cancer itself. She is specifically widening the focus of her research to include lymphedema care in head and neck cancer survivors.