A new orthopaedic surgery program at Vanderbilt University Medical Center is combining foot and ankle expertise with trauma surgery to restore lower limbs that have deteriorated from bone loss, infection or deformity.
Part of Vanderbilt’s Orthopaedic Limb Loss Program, the dedicated lower limb effort is led by Bethany Gallagher, M.D., an assistant professor of orthopaedic surgery at Vanderbilt, and Lieutenant Colonel Daniel Stinner, M.D., an associate professor of orthopaedic surgery and active-duty Army surgeon. Stinner’s work supports the Military-Civilian Partnership between Vanderbilt and Army Medicine.
Severe lower limb injuries require multispecialty expertise and a high level of continuing care. Vanderbilt is a level 1 trauma center with specialists in imaging, infectious diseases, plastic surgery, prosthetics and other disciplines readily at hand.
“Our primary goal is restoration of function, which encompasses so much more than surgical treatment,” Gallagher said. “With these resources close by, we are able to swiftly and appropriately manage these complex injuries with our team.”
“Limb restoration patients often require frequent clinic visits to assess wound and bone healing with adjustments made in the treatment plan if necessary,” Stinner added. “Most orthopaedic practices don’t have the resources available to deliver this type of care.”
Salvage vs. Amputation
Lower limb deterioration may result from multiple causes, including severe trauma injury, osteomyelitis, diabetes or peripheral vascular disease. There are management standards for each condition; however, when viability or function of the limb is severely threatened, the decision to amputate or attempt salvage becomes the primary challenge.
“Our primary goal is restoration of function, which encompasses so much more than surgical treatment.”
Salvage versus amputation decisions are based on the degree of nerve injury, ischemia, soft-tissue contamination, skeletal damage, shock and a patient’s age (also known as the NISSA index). This and other indices – including the Predictive Salvage Index, Mangled Extremity Severity Score, and Limb Salvage Index – have been developed to help surgeons and care teams make the salvage decision.
“Limb salvage is complex and the decision to salvage a deteriorating limb is multifactorial,” Gallagher said. “Every restoration requires unique strategies.”
Split-second Decisions
Trauma is the most frequent cause for lower limb salvage surgery and demands quick, careful assessment. As a military orthopaedic trauma surgeon, Stinner helps train Army orthopaedic surgeons to perform combat-relevant surgical procedures. In severe traumatic injuries, he says, the cases surgeons encounter in many busy level 1 trauma centers are much like what military surgeons see on the battlefield.
Standard of care for trauma is careful debridement with stabilization and prompt wound coverage to prevent failure, infection and improve the bone healing environment. Once initial stabilization is complete, the team plans more definitive management if needed, Stinner said.
Imaging to Inform Diagnosis and Treatment
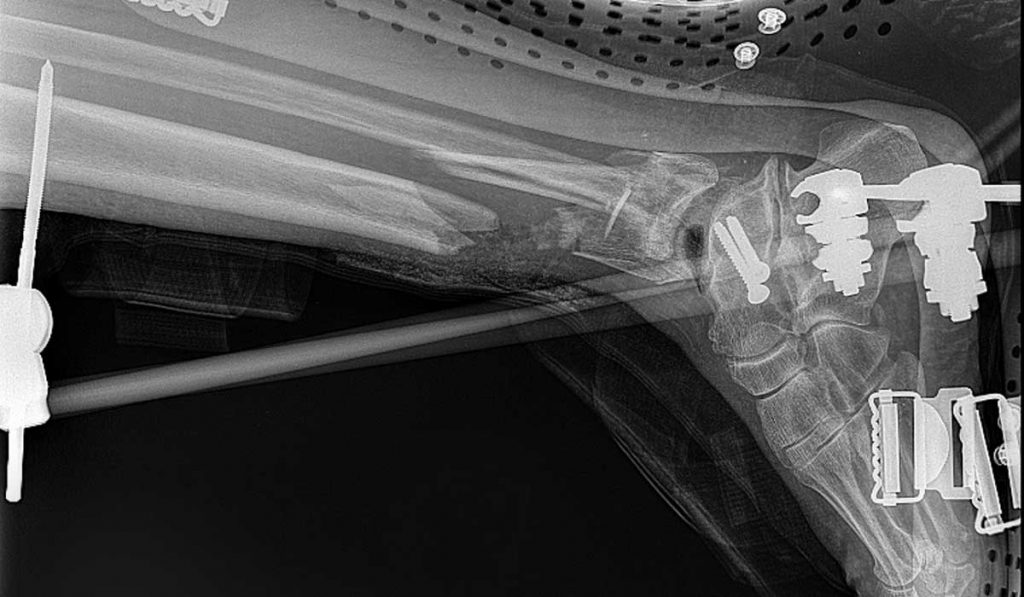
Whether the patient presents through the ED or as a referral, the physician spends significant time obtaining and reviewing appropriate imaging.
“A unique and powerful tool in the new program is distraction osteogenesis, which provides the ability to remove the compromised bone and essentially grow or transport bone into the defect.”
“CT scans are critical in planning stages for acute fracture management as well as planning for deformity correction or bone resection in severe cases of infection,” Gallagher explained. “They also allow us to determine healing of the bones as time goes on and as patients are preparing to walk again.”
If there is concern for deep bone infection either at initial consultation or as the treatment evolves, the orthopaedist consults a team of infectious disease physicians that focus specifically on bone infections. Similarly, plastic surgeons are consulted to provide skin and muscle coverage critical for bone healing in catastrophic injuries or infections.
Surgical Strategies
Once the plan has been established and thoroughly discussed with the patient, the physician moves forward with surgical intervention. The orthopaedics team at Vanderbilt employs personalized microsurgical strategies including complex fusions, bone allografting, deformity correction and ankle arthrodesis to restore function.
“A unique and powerful tool in the new program is distraction osteogenesis, which provides the ability to remove the compromised bone and essentially grow or transport bone into the defect,” Gallagher said. “This is time intensive and requires detailed planning by the physician but can be an opportunity to salvage a limb thought only to be best treated with amputation.”
Facilitating Recovery
The new lower limb restoration program joins several other Vanderbilt initiatives focused on limb restoration including upper extremity limb salvage and limb loss pain, a limb loss care clinic and the Center for Rehabilitation Engineering and Assistive Technology (CREATE).
“Vanderbilt has everything – clinical expertise, ancillary support and computer-aided prosthetic design,” Gallagher said. “Working with such a qualified team gives patients a comfort level and facilitates recovery.”