The U.S. Preventive Services Task Force (USPSTF) has formally recommended changes to lung cancer screening guidelines in an effort to reduce outcome disparities between African American and white patients.
The decision is based in part on research led by Melinda Aldrich, Ph.D., an associate professor of medicine at Vanderbilt University Medical Center. The research team included Kim Sandler, M.D., an assistant professor of radiology and radiological sciences and co-director of the Vanderbilt Lung Screening Program.
“Overall, our goal is to equalize the performance of lung cancer screening for African American smokers and narrow the gap in health disparities between them and other groups. Screening guidelines should be equitable,” Aldrich said.
Added Sandler, “The adjustment of these guidelines is an extremely important step that will allow us to screen earlier in order to continue to improve morbidity and mortality from lung cancer.”
Smoking Risks Vary Among Racial Groups
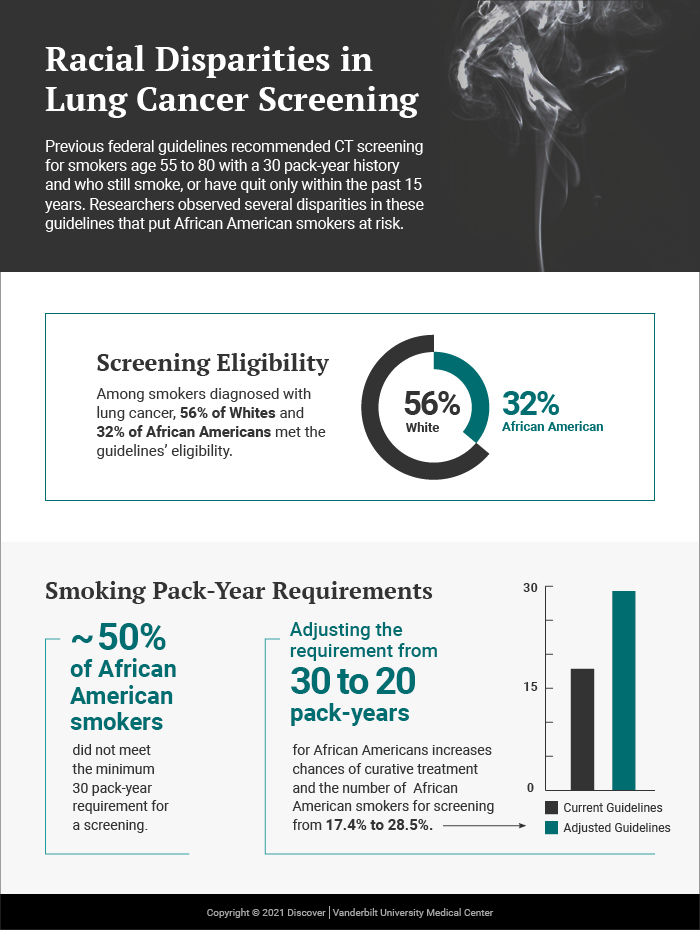
The previous guidelines recommended CT screening for smokers age 55 to 80 with a 30 pack-year history who still smoke – or quit only within the past 15 years. Landmark research by the Vanderbilt team published in JAMA Oncology revealed that only 32 percent of African American patients with lung cancer would have qualified for screening versus 56 percent of white patients.
“Our goal is to equalize the performance of lung cancer screening for African American smokers and narrow the gap in health disparities.”
The Vanderbilt study highlighted specific smoking patterns and how they influenced screening eligibility.
“African American smokers tend to smoke fewer cigarettes overall as compared to white smokers, but their lung cancer risk remains high,” Aldrich said, adding that the previous guidelines failed to address this discrepancy.
Uncovering Multiple Disparities
In total, the researchers analyzed data from 48,364 “ever-smokers” enrolled in the Southern Community Cohort Study, among whom 1,269 patients developed lung cancer. African American smokers comprised 67 percent of the overall cohort. The study was one of the largest evaluations ever done of the USPSTF lung cancer screening guidelines in African American smokers.
The researchers collected demographic information alongside data on smoking habits and history. Nearly half of African Americans diagnosed with lung cancer did not meet the minimum 30 pack-year requirement for screening, while only 16 percent of white lung cancer patients failed to reach that minimum. The authors noted that for African American smokers, adjusting the requirement from 30 to 20 pack-years would increase the number of those eligible for screening from 17.4 to 28.5 percent. This lower pack-year threshold is now embedded in the new guidelines.
Across both racial groups, large proportions of smokers who later developed lung cancer did not meet age requirements for screening (24 percent of African American patients; 19 percent of white patients). Thus, the lower age requirement in the updated guidelines (age 50) could have widespread benefits – particularly for African Americans who often develop lung cancer at an earlier age than other groups.
Going Beyond Screening
Revising the USPSTF guidelines is a key step to improving lung cancer screening access for African American smokers, since the guidelines inform how insurance companies determine CT scan coverage, say the researchers. Screening for the disease has been insufficient, especially compared to levels of screening for breast and colorectal cancer.
Sandler and Aldrich note that reluctance is another significant barrier to lung screening among patients of all racial and ethnic groups. “There’s a lot of stigma with lung cancer screening,” Sandler said. “Patients feel responsible for the exposure.”
“The recommendations put forth by the USPSTF are a step forward in the right direction,” Aldrich said, “However, more work is needed to address disparities that still likely exist.”
Toward that aim, Aldrich is working with Christine Lovly, M.D., Ingram Professor of Cancer Research at Vanderbilt, on a multi-institution study designed to improve participation of communities of color in lung cancer clinical trials.
“Geographic and racial/ethnic disparities occur in cancer outcomes, including lung cancer,” Aldrich said. “To ensure equity in health outcomes across diverse communities, it is time we fix the lack of racial/ethnic and geographic diversity in clinical trials.”