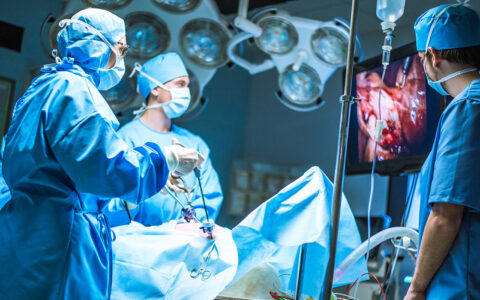
A new cardiac catheterization laboratory has opened at Monroe Carell Jr. Children’s Hospital at Vanderbilt, helping to address a growing patient volume and demand for complex procedures.
The interventional laboratory is directly connected to a brand-new post-anesthesia care unit, as well. In total, the 10-bed addition required nearly a dozen new specialty staff hires.
“This lab has about twice the space of our existing area,” said director Dana Janssen, M.D., an associate professor of pediatrics at Vanderbilt. “The new space will allow us to not only serve our cardiac patients in a timely fashion, but they will have a place dedicated to their care and recovery.”
Space for Collaboration
“The new area is ideal for the care of our complex patients,” added Thomas Doyle, M.D., an interventional cardiologist at Children’s Hospital. “The intake area, recovery room and catheterization laboratory are within feet of each other and only a few steps from our work area. The entire team of nurses, cardiologists and anesthesiologists can be available almost immediately for any issues that arise.”
“The new space will allow us to not only serve our cardiac patients in a timely fashion, but they will have a place dedicated to their care and recovery.”
Increased square footage is particularly beneficial for patients needing more support, Doyle says, such as patients on extracorporeal membrane oxygenation who require a team of perfusionists, or in particularly complex cases where an additional surgical team would be required.
Hybrid Capabilities
The new catheterization laboratory is versatile, designed for both pediatric and adult patients. Most notably, it now equips Children’s Hospital for hybrid procedures that combine surgical approaches with simultaneous catheter-based interventions.
Said Janssen, “With the hybrid component, it meets all the requirements for it to be a fully working operating room. A hybrid room allows us to serve patients who don’t have a straightforward approach either surgically or in the cath lab.”
Hybrid capability may be particularly beneficial for congenital heart disease patients with complex anatomy. For example, a Norwood procedure, the primary palliative procedure for certain children with a single ventricle defect, is typically performed surgically.
“We actually have patented devices that are being studied now to make the hybrid Norwood a completely cath-based procedure,” Janssen said. “Our hope is that our devices will prevent newborns from needing the first stage of surgery. Thus, they will only have two heart surgeries rather than three at a minimum, and the first will happen at 4-6 months of age rather than the first 1-2 weeks of life.”
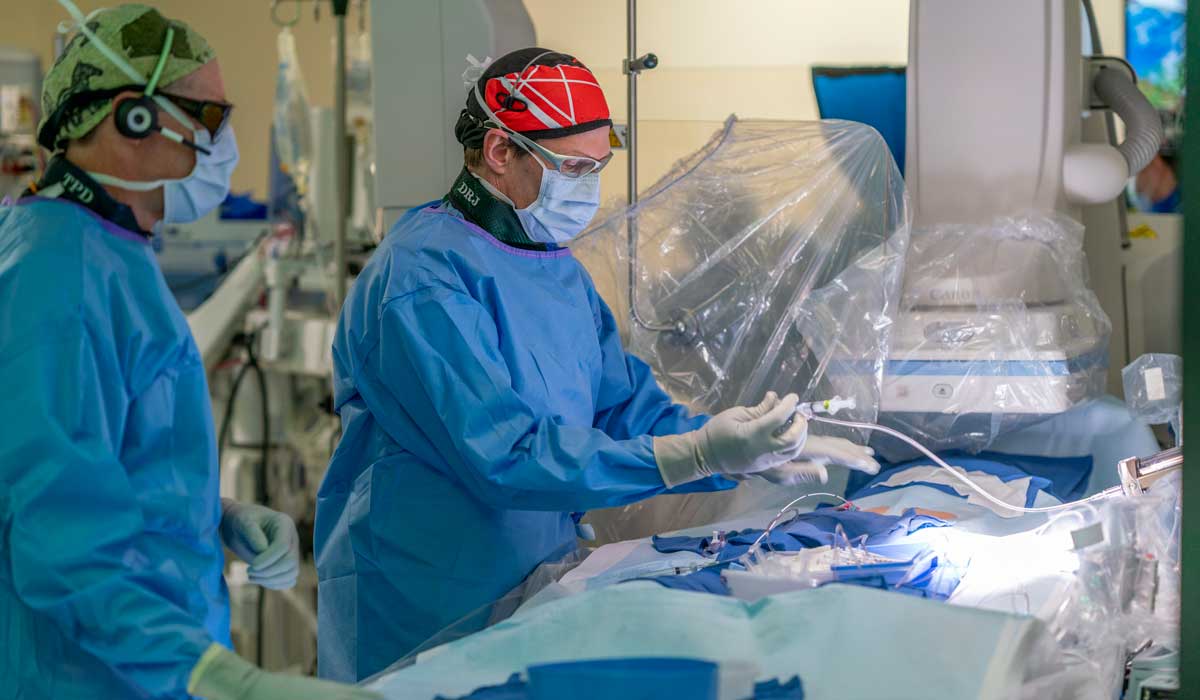
Improved Technology
A Canon AlphenixTM Biplane with high definition panels in the new laboratory elevates imaging capabilities. For some procedures, the system offers higher 3D image quality with the same or less radiation than previously required, Janssen said.
The space also incorporates audio and video link technology to enable the cardiac ICU and non-invasive imaging teams to have direct contact with the catheterization lab and discuss cases without having to leave their clinical areas. This real-time communication enables a seamless handoff and collaboration between procedures.
An Expanded Specialty Team
“I am excited about the new space, the high-tech equipment and the ability to meet the growing needs of our patient population,” Janssen said, adding that Sara Hightower, R.N., who was instrumental in launching the new laboratory at Vanderbilt, will continue to serve as clinical staff leader.
“Our hope is that our devices will prevent newborns from needing the first stage of surgery.”
The expanded capabilities will help address Vanderbilt’s growing patient population. In 2020, Vanderbilt performed more heart transplants than any other facility worldwide. All the post-transplant biopsies required catheterization.
Janssen and colleagues also share space with the electrophysiology laboratory at Children’s Hospital. Together, the team completed approximately 1,200 cases last year – 800 of which were catheterization cases. The majority were patients with congenital heart disease.
“Now we have an expanded ability to perform the procedures we need to, when we need to, without disrupting or cancelling other procedures. This minimizes the risk of a last-minute cancellation of a procedure for a family that has had to go to great lengths to come to Children’s Hospital,” Doyle said.
“This is complete care given by a dedicated team – all in one location,” Janssen added. “The dedicated recovery area allows for a small team of nurses to care for the patient before and after their procedure. The same nurse that does the intake when the patient arrives will be the nurse who cares for them after the procedure. This improves safety during handovers.”