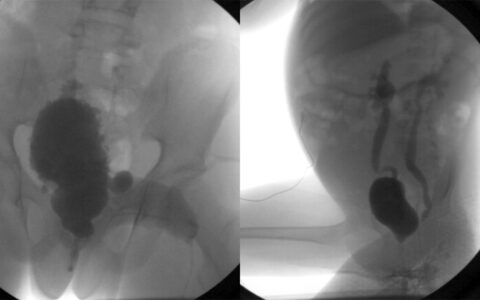
A study of the bladder management and outcomes of participants in the National Spina Bifida Patient Registry, published in The Journal of Urology, has given researchers a foundation for new guidelines that help determine realistic goals and best treatments for younger spina bifida (SB) patients.
The transition to adult care for spina bifida patients is of critical importance. Continence in adult patients is significantly associated with higher education levels, higher levels of employment, and having private health insurance, the study found.
“Spina bifida care today is no longer just about survival,” said Stacy Tanaka, M.D., a professor in the Division of Pediatric Urologic Surgery at Monroe Carell Jr. Children’s Hospital at Vanderbilt, and author on the study and latest guidelines. “It’s about figuring out how to support individuals to live the lives they want to lead.”
Adolescent Bladder Management
The Journal of Urology study was the largest of its kind to date and included 5,250 participants with spina bifida grouped into three categories, including 1,993 school-age children (5-11 years), 1,885 adolescents (12-19 years), and 1,372 adults (20 years or older).
The multicenter research group found bladder continence increased with age in spina bifida patients: 37 percent in school-age children, 47 percent in adolescents, and 48 percent in adults. The most common form of bladder management by a wide margin was clean intermittent catherization, which also increased with age to include more than 75 percent of adults. Half of all participants, but particularly young children, used antimuscarinic medication. Antibiotic use was fairly low and increased with age.
“Spina bifida care today is no longer just about survival, it’s about figuring out how to support individuals to live the lives they want to lead.”
The percentage of patients with no bladder management decreased with age, with a sharp drop in the transition from school-age to adolescent groups (12 to 6 percent). Adolescents were the most likely study group to have undergone bladder outlet surgery, which researchers stated could reflect a recent turn toward more aggressive efforts to help SB patients achieve continence.
“With increased focus on transition care, we’ve also been engaging adolescents more to help prepare them to assume responsibility for their own health,” said Tanaka, who is also the director of Vanderbilt’s Spina Bifida Clinic.
Early Intervention for Long-term Success
The data suggest the transition period as children become teenagers is critical for implementing bladder management. As management continues into adulthood, it will be important for those adolescents to have the expectation that treatment is likely to continue and will be an ongoing process, Tanaka says.
The findings align with the latest SB care guidelines, which emphasize three primary goals:
- Maintain normal renal function throughout the lifespan.
- Achieve urinary continence as early as socially acceptable.
- Maximize urologic independence.
Tanaka says subpopulations require additional considerations. Further data analyses showed myelomeningocele (MMC) SB patients had much lower levels of continence, though continence did improve with age, maxing out at 46 percent in adults. Overall, 64 percent of non-MMC SB patients achieved continence, with adolescents showing the highest rates.
“With increased focus on transition care, we’ve also been engaging adolescents more to help prepare them to assume responsibility for their own health.”
Socioeconomic data revealed strong ties between successful management of SB and other benefits, with statistically significant associations between early bladder continence and higher education and employment levels. As a whole the report underscores the importance of patients knowing all their options to achieve continence before they reach adulthood.
“These data are helpful not only to evaluate current care, but also to provide realistic expectations to younger individuals about future management and outcomes,” wrote the authors.