A recent study published in Neurology and Urodynamics by a team of researchers at Vanderbilt University Medical Center, led by Abby Taylor, M.D., an assistant professor of urology, shows that pelvic floor biofeedback therapy (PFBT) can be an effective teaching tool to improve quality of life for patients with lower urinary tract symptoms (LUTS) who have not shown improvement with standard urotherapy.
PFBT, which uses surface electrodes to monitor the pelvic floor musculature, allows patients to learn how to consciously control those muscles during voiding. It offers a potential solution for the more difficult patients with LUTS, one of the most common referrals to a pediatric urologist. The benefits of successful PFBT include improvements in urinary incontinence, bladder emptying, number of urinary tract infections, and vesicoureteral reflex.
“Children with urinary problems make up a large part of our practice in pediatric urology,” said Douglass Clayton, M.D., an associate professor of urology at Vanderbilt, the senior author on the study. “These children suffer from significant problems, and pelvic floor biofeedback therapy is a tool we can use to make their lives better.”
Majority of Patients Report Decreased Symptoms
Monroe Carell Jr. Children’s Hospital at Vanderbilt introduced PFBT into practice in 2012. To determine best practice and understand the results of the treatment since its introduction, Taylor and her team retrospectively reviewed the charts of all children undergoing PFBT from August 2012 to July 2016. The study assessed PFBT’s effectiveness in treating patients with refractory LUTS and an inappropriately active EMG during voiding.
EMG quieting and improved symptoms as determined by the validated Vancouver bladder bowel dysfunction (BBD) symptom score questionnaire were used to measure the efficacy of PFBT in treatment.
Of the 229 patients who had participated in PFBT treatment in the study period, 64 met inclusion criteria— defined as female patients, six years of age or older at first treatment, who had completed two or more PFBT sessions, shown persistent LUTS refractory to standard urotherapy with an active EMG during voiding, and had completed two BBD questionnaires.
“These data, even though they were retrospective, show us that with dedicated treatment plans we can have an objective effect on how these children empty their bladders, which we hope will translate to better quality of life.”
Results of the study showed that 31 percent of patients achieved EMG quieting from PFBT identified as “responders” versus the 69 percent “non-responders,” and that 80 percent reported a decrease in BBD symptom scores.
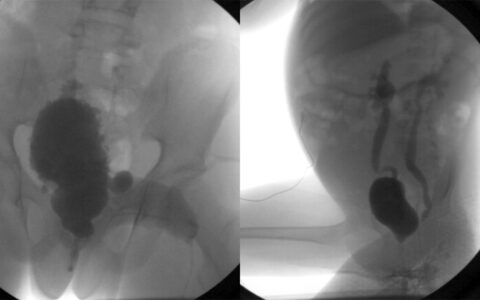
In addition, the percentage of patients exhibiting a normal uroflow pattern increased significantly post treatment. Normal bell-shaped uroflow patterns were shown in 17 percent of patients before treatment and 47 percent after treatment. Staccato patterns were shown in 52 percent of patients before treatment, decreasing to just 22 percent after.
“These data, even though they were retrospective, show us that with dedicated treatment plans we can have an objective effect on how these children empty their bladders, which we hope will translate to better quality of life,” Clayton said.
Encouraging Results, Further Research
Previous data has tied poorer quality of life to higher BBD symptom scores, suggesting that PFBT has improved qualityof life for the patients who reported a decrease in symptom scores. The “responders” in the study reported a 47 percent decrease in scores, and “non-responders” reported a 23 percent decrease.
The 69 percent of patients who did not achieve EMG quieting were on average nearly two years younger than those who did, leading researchers to hypothesize that younger children are less likely to cooperate with EMG techniques, which can lead to false positives of increased pelvic floor activity.
Although only 31 percent of patients demonstrated an improvement in EMG activity following a minimum of two PFBT sessions, the significant decrease in symptom scores and reduction in staccato uroflow patterns are encouraging for the effectiveness of PFBT in treating one of urology’s greatest areas of need.
“This study was important because it helped us see that our pelvic floor biofeedback program could have real results,” Clayton said. “It led us to implement a prospective study designed by Dr. Taylor which has already launched in our division to study PFBT in greater detail.”