Asthma is the leading chronic disease among children, affecting up to 8.4 percent of children in the United States. Childhood asthma incidence is also rising across the globe at rates not solely attributable to genetics. As a result, modifiable risk factors have become increasingly critical to help guide physicians, scientists and policymakers toward effective interventions.
“80 percent of asthma onset is during childhood, and there are many significant factors in disease development,” said Tina Hartert, M.D., Director of the Asthma Research Center at Vanderbilt University Medical Center. “We need to think about asthma in the way we’ve approached cardiovascular disease, trying to modify multiple risk factors through a multifaceted approach. With asthma, we’ll need a similar approach targeting pregnant women, infants and children.”
Hartert along with Andrew Abreo, M.D., a clinical fellow at the Asthma Research Center, recently published a large-scale summary of 32 meta-analyses to identify the most impactful risk factors for child asthma at a population level, and to estimate the effects of potential targeted interventions. The study is among the first to summarize such a huge amount of asthma data.
Individual Risk Factors and Asthma Development
To evaluate risk factor prevalence and impact on child asthma in the U.S. population, Vanderbilt researchers used data from meta-analyses of relevant studies conducted between 1990 and 2017.1 The contribution of specific risk factors to the burden of asthma in a population was quantified using population attributable fraction. In total, the analysis considered 31 risk factors across four age exposure windows: prenatal, infancy, 1 to 5 years, and 5 to 13 years.
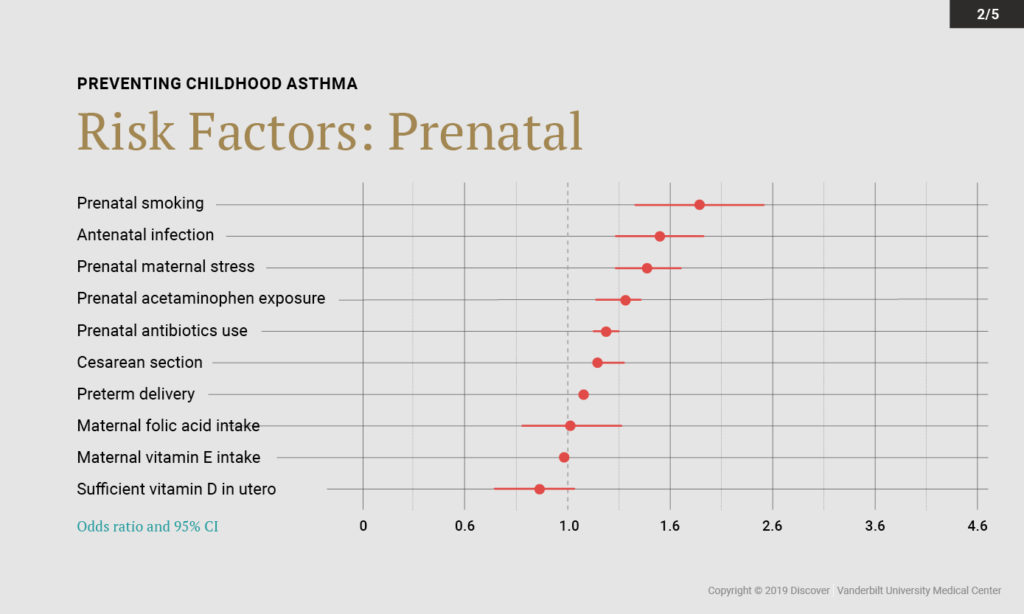
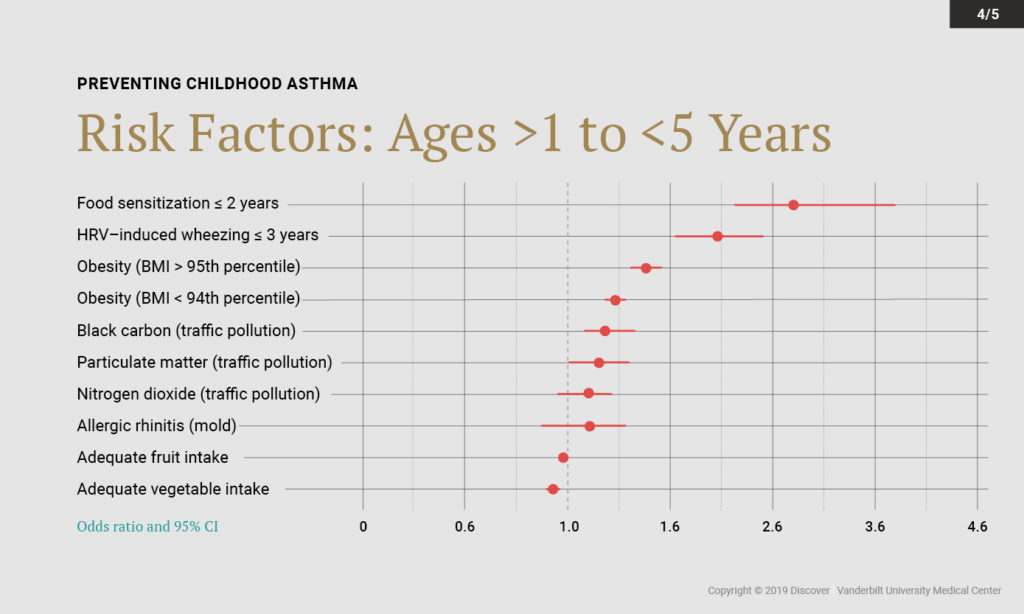
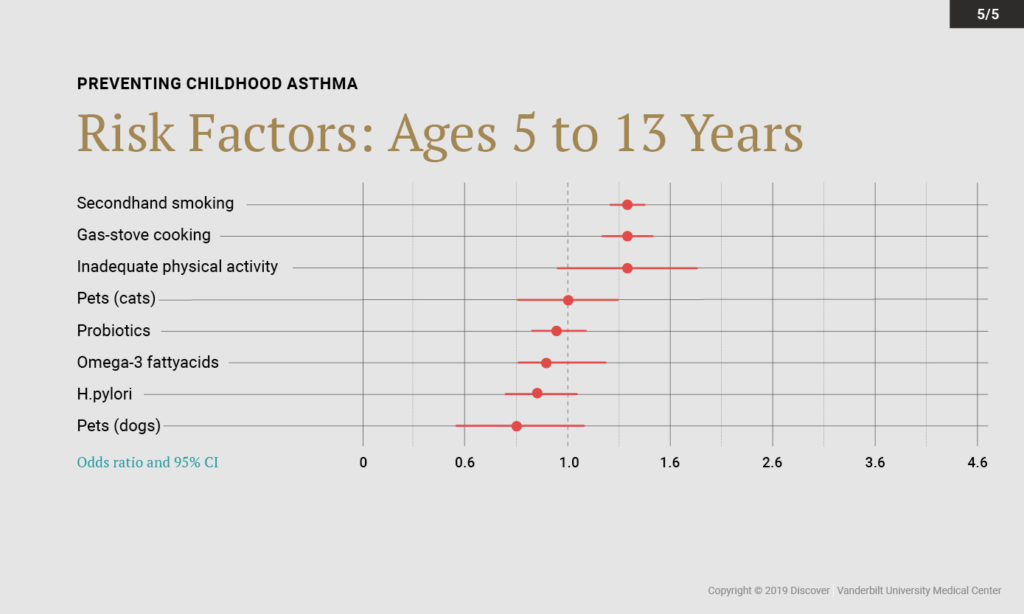
By combining results across studies, the researchers identified a number of modifiable prenatal and early childhood risk factors with a high population attributable fraction. These risk factors – including acute respiratory illness, cesarean delivery, and secondhand smoke exposure – were found to have a large impact on childhood asthma development.
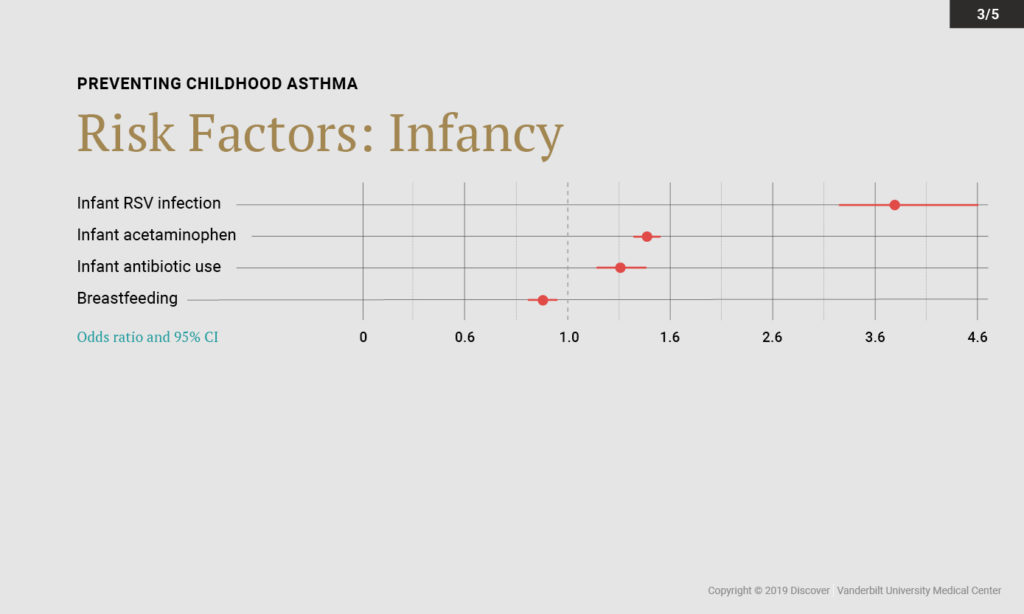
Two factors emerged as potentially protective against development of childhood asthma: breastfeeding and sufficient prenatal vitamin D concentrations. “We’re particularly interested in dietary factors,” Hartert said. “Diet is modifiable and safe in relatively vulnerable populations—pregnant women and young children.”
Vaccination against RSV may also be critical, Hartert explained, particularly in low- and middle-income countries where there is the greatest mortality from RSV.
“We take for granted in the US that if we have an effective vaccine for RSV, every child will receive it,” she said. That’s not what happens everywhere. RSV results in the greatest morbidity and mortality in the first year of life; if we can show it also contributes to later respiratory diseases and asthma, we’re more likely to get that vaccine distributed internationally because it could have both short and long-term benefits.”
Merging Population Strategy and Personalized Medicine
“At a population level, we need to be targeting the risk factors that are ubiquitous, modifiable and contribute to the largest proportion of disease development.”
“We don’t yet know if certain individuals will benefit more than others from risk factor modification,” Hartert said. “More targeted studies need to pinpoint the host genetic risk factors and modifiable risk factors that make a certain child more or less likely to develop asthma. Meanwhile, at a population level, we need to be targeting the risk factors that are ubiquitous, modifiable and contribute to the largest proportion of disease development.”
Vanderbilt leads a range of studies across this spectrum. The Center for Asthma Research employs a unique translational model to engage its individual patients in innovative research, while Hartert’s research team is also tracking large-cohort data sets spanning the region, state of Tennessee and the US. The Center also partners with the World Health Organization (WHO) to study the role of RSV in asthma development internationally.
“Early diagnosis and treatment of chronic respiratory diseases—asthma prevention—is clearly recognized as a public health priority, not only in the United States, but worldwide, and by the WHO. This is a major research and policy priority,” Hartert said.