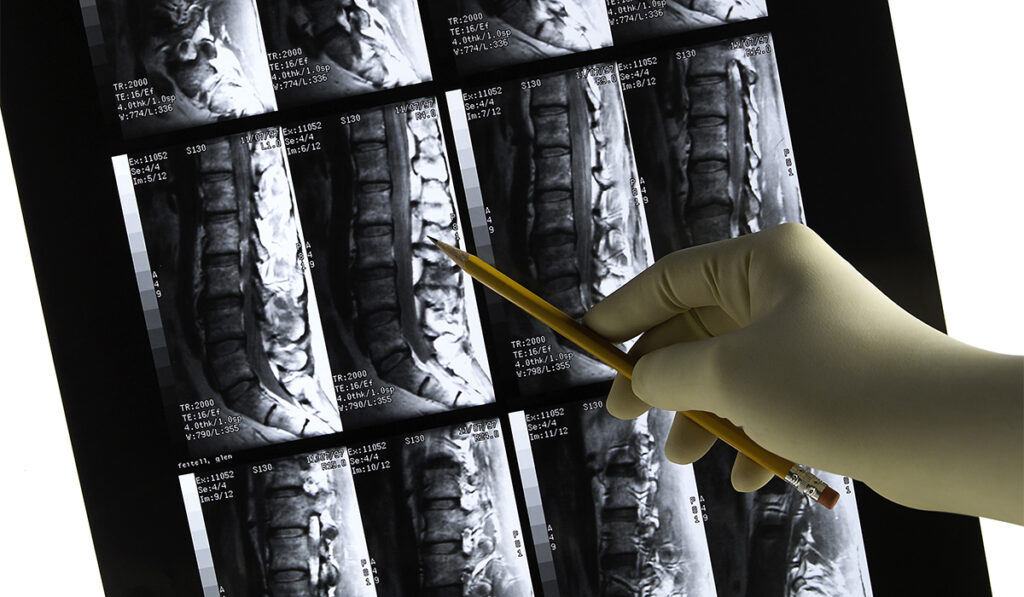
In recent years, improvements in technology and surgical techniques have been key to advancing minimally invasive alternatives to traditional spine surgeries. Interest is particularly high for endoscopic spine surgery, as some procedures can be done in an outpatient setting and without the need for general anesthesia.
Raymond Gardocki, M.D., an associate professor of orthopaedic surgery at Vanderbilt University Medical Center, is an expert in this innovative procedure and provides patients at the Vanderbilt Spine Center the option to be treated with ultra-minimally invasive spine surgery if their condition allows.
“Endoscopic spine procedures add value for the patient because they have less pain and a faster recovery,” Gardocki said. ”They add value to society because they reduce ancillary costs and overall health care burden.”
“Few surgeons in the U.S. can boast Dr. Gardocki’s experience with endoscopic spinal procedures,” added Jacob Schwarz, M.D., an assistant professor of neurological surgery at Vanderbilt and executive medical director of the Vanderbilt Spine Center. “For carefully selected patients, these techniques offer exciting opportunities to improve their troublesome symptoms with minimal recovery time.”
Endoscopic Spine Surgery
In contrast to traditional spine surgeries with larger, open incisions, endoscopic spine surgeries cause less damage to surrounding muscle and soft tissues, Gardocki says, which means reduced post-surgery pain and inflammation.
“Patients do not need narcotic prescriptions after un-instrumented endoscopic spine procedures because they are recovering from the underlying pathology rather than the surgical approach,” Gardocki said.
In addition, Gardocki performs many endoscopic spine surgeries under moderate sedation in the outpatient setting, avoiding some of the issues of general anesthesia, like postoperative nausea and delirium.
“Patients do not need narcotic prescriptions after un-instrumented endoscopic spine procedures because they are recovering from the underlying pathology rather than the surgical approach.”
Training a New Generation
To expand access to endoscopic spine surgeries and other technically advanced surgical procedures, Gardocki has helped launch an Orthopaedic Spine Fellowship at Vanderbilt to train early-career surgeons.
“We are offering trainees a skull-to-sacrum, high-volume experience,” Gardocki said.
Fellows will be immersed in evaluation and surgical management of degenerative, deformity, oncologic, infectious, and traumatic conditions of the full spine. In addition to exposure to minimally invasive and endoscopic spine surgery, fellows will be introduced to other cutting-edge procedures such as osteotomies for spinal deformity, motion-preserving surgery, and en bloc spondylectomy.
“There are few accredited spine fellowships with endoscopic surgeons on staff in the U.S.,” Gardocki said. “We expect to attract emerging physicians seeking to start their careers with strong exposure to minimally invasive spine surgery.”
COVID-19 Increases Demand
Gardocki explains that patients have been seeking outpatient spine procedures for a long time, reminiscent of the rush of demand for outpatient surgery for total joint replacements.
Now, with the COVID-19 pandemic heightening patient concerns about hospital access and safety, the need for greater access to endoscopic options has only intensified. “In this moment, it’s huge for us to be able to offer an awake, endoscopic procedure,” Gardocki said.