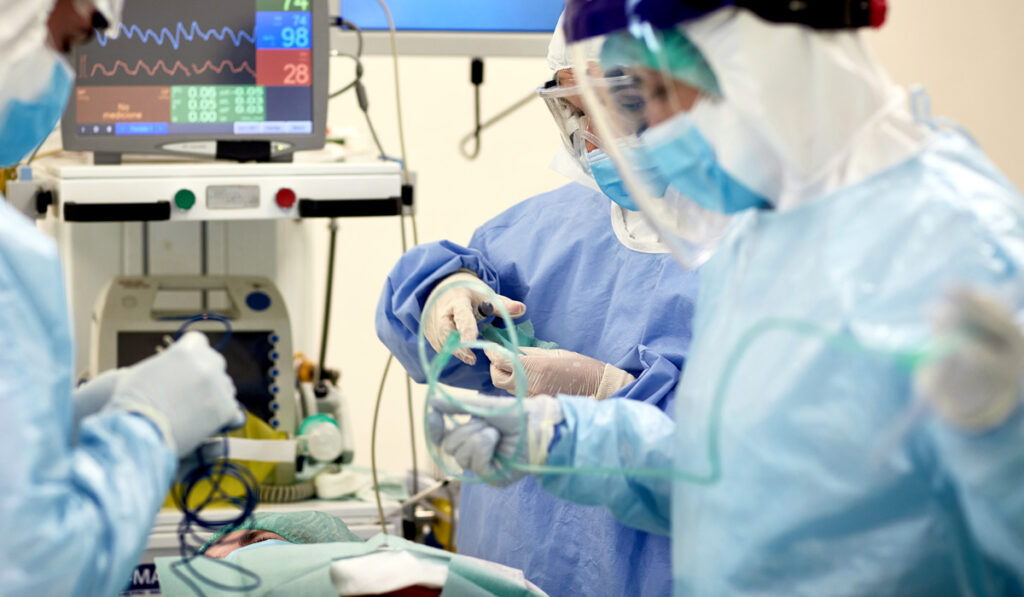
A transplant team at Vanderbilt University Medical Center has performed the first combined heart-lung transplantation on a patient after a COVID-19 diagnosis. The 41-year-old patient had ongoing cardiomyopathy that was compounded by severe lung damage from COVID-19 in June. He arrived at Vanderbilt critically ill.
Leaders of the transplant team Ashish Shah, M.D., chair of the Department of Cardiac Surgery, and Matthew Bacchetta, M.D., associate chair of the Department of Thoracic Surgery, recognized that dual transplantation was the patient’s only hope. “The patient had decompensated lungs. He had been in and out of the hospital back in his home state and was now slipping fast. By the time we operated on him, his heart was really done,” Shah said.
Following the transplantation of a quality heart and lung block from a hepatitis C-positive donor, the patient stabilized within days. As of late October, he is out of the ICU and recovering in the hospital. He has tested hepatitis C and COVID-19 negative.
“Given his relatively young age and overall organ health, his prospects are good,” Bacchetta said.
A Unique Case for Dual Transplant
Vanderbilt’s last heart-lung transplantation was performed in 2006. Shah says the indications for dual transplantation have narrowed with the discovery of how compromised hearts often recover after lung transplantation alone. This patient, with end-stage heart and lung disease, fit the narrow criteria for a dual transplant.
Shah and Bacchetta’s decision to perform the procedure together broke precedent at Vanderbilt. Bacchetta says the pair’s success leaned on rapid coordination between the ICU, heart, lung and anesthesia teams on pre-op, post-op and long-term care plans.
“We drilled down on every step, from the types of donors we would consider to the organ procurement process, the technical aspects of the surgery, intraoperative management and post-operative care,” Bacchetta said.
“We prepared in one week for this surgery, but it represented five years of foundational work – putting together the right elements of what are highly skilled and dedicated teams. We just had to fine-tune the logistics for a heart-lung transplant and for this particular patient,” Shah said.
Managing Perioperative Risks
Bleeding risk is always paramount in a transplantation, but Shah says the most critical moment was when they reperfused the organs. “Despite our best efforts, one or both organs could fail as a result of being on ice for several hours. We had to manage the process very carefully to avoid those problems.”
Timing of heart-lung support was also pivotal. A weak heart is particularly vulnerable to fail under the pressure to support the work of the lungs while they are cut away from scar tissue and adhesions. “Not long after we started, it became apparent that the patient’s heart was rapidly deteriorating and he would not tolerate further dissection,” Bacchetta said. “We decided together to use the heart-lung machine a bit early.”
“We prepared in one week for this surgery, but it represented five years of foundational work.”
Once the organs were implanted, blood flow restored, and the function of both heart and lungs stable, the patient was safely weaned off the bypass machine. The long road to recovery began.
The Somber Aftermath of COVID-19
If not for COVID-19, Shah and Bacchetta say the patient might have survived decades without intervention, or he might have eventually become a candidate for heart transplant. His COVID-19 infection rapidly changed his prospects.
“We don’t believe he was that unwell prior to COVID-19, but the infection was severe. This probably accelerated his heart disease – and it certainly wrecked his lungs,” Shah said.
Shah says the case is a sobering reminder that we don’t yet fully understand how some patients respond to COVID-19 infection. “It highlights that we are destined to see more chronic consequences of the virus on the lungs, unfortunately,” he said.