As with every facet of patient care, the COVID-19 pandemic has had a profound impact on the U.S. practice of transplantation. According to the American Society of Transplant Surgeons (ASTS), deceased donation has declined, living donor transplants have been greatly curtailed and multiple programs have been suspended. Due to infection risk, ASTS strongly recommends against travel for both patients and organ transplant teams.
The Vanderbilt Transplant Center, a leading provider of organ transplantation in the Southeast, is collaborating with Tennessee Donor Services (TDS) in a model program to facilitate the organ procurement process for outside centers.
“When COVID-19 hit, surgical staff couldn’t travel safely to retrieve organs,” said Seth Karp, M.D., surgeon-in-chief at Vanderbilt University Medical Center and director of the Vanderbilt Transplant Center. “This program establishes a vital link to recipient centers by preparing and transporting organs to them.”
“This program establishes a vital link to recipient centers by preparing and transporting organs to them.”
Managing Transmission Risk
Acquisition and spread of SARS‐CoV‐2 has been reported from both live and deceased donations. Transmission may be affected by several factors: epidemiology, incubation period, degree of viremia and viability of the virus in blood and organs.
Additionally, because organ transplant recipients require immunosuppression, patients may be more vulnerable to contracting the virus and may have more intense and prolonged viral shedding, potentially increasing the transmission risk.
“All transplant programs should assess risk based on their unique circumstances,” Karp said. “The goal is to protect both patients and staff.”
Until more is known, ASTS advocates that organs from COVID-19-positive donors should not be recovered or transplanted. COVID-19 testing should be performed on all deceased donors, acknowledging that COVID-19 testing is rapidly evolving. Living donors for emergent donation should be decided on a case-by-case basis.
Impact on Organ Donation
While total donations this year have tracked with 2019, transplant surgeries decreased significantly in the weeks between March 3 and May 8, according to United Network for Organ Sharing data. Because of hospital restrictions on surgery, living donations dropped significantly more than deceased donations.
“In the first six weeks of the pandemic, we faced many challenges and saw a significant drop in donation,” said Jill Grandas, TDS executive director. “Hospitalizations were down, and more people died at home for fear of going to the hospital.”
A Model for Organ Retrieval
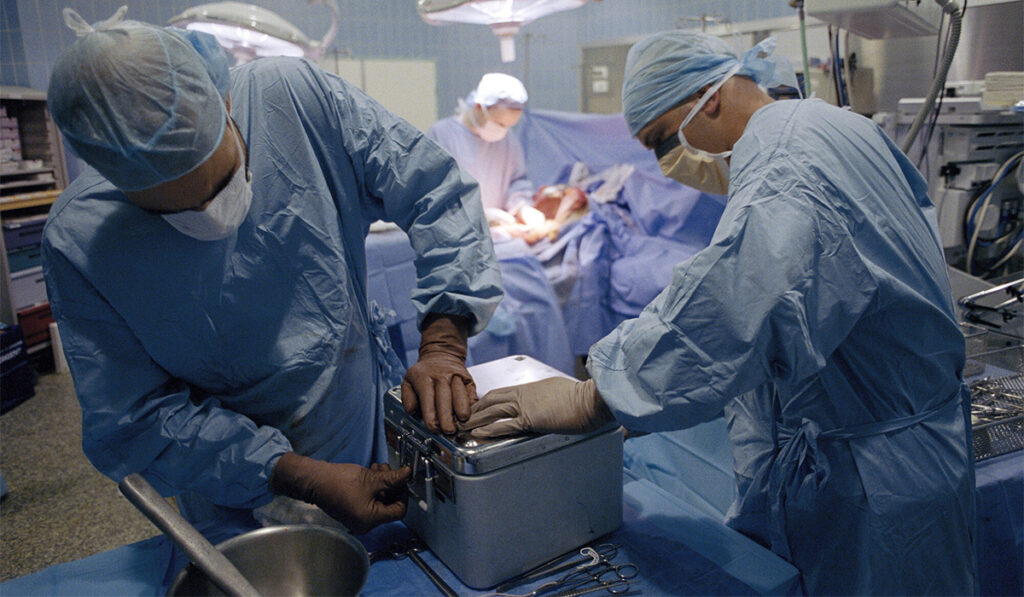
To limit patient and staff exposure to the virus, outside surgical teams who would normally travel to Vanderbilt to retrieve organs do not make the trip. Instead, for organs allocated to outside centers, TDS coordinates with Vanderbilt transplant surgeons, organ procurement coordinators, OR staff, preservationists and pharmacists to prepare the organs and arrange for transport.
“It’s a great example of many people coming together to problem solve,” said Dawn Eck, ACNP-BC, APN manager of thoracic transplant and organ procurement at Vanderbilt. “It has made us reexamine how we might do things differently in the future beyond COVID.”
“It has made us reexamine how we might do things differently in the future beyond COVID.”
Karp views the procurement program as Vanderbilt’s responsibility to the community. “COVID has made this service more essential than ever,” he said. “We may be living with this virus for months, even years, to come.”