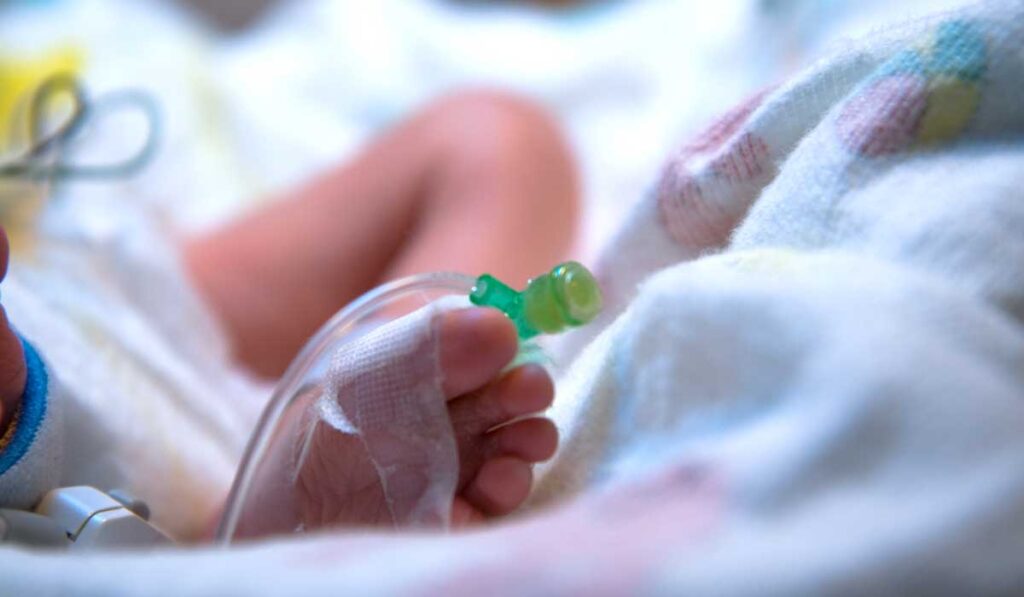
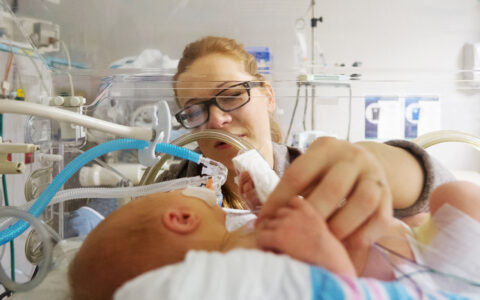
A recently completed phase 3 clinical trial assessed the safety and efficacy of SMOFlipid, a new lipid emulsion formulation, as a source of nutrition for hospitalized neonates and infants requiring total parenteral nutrition. Monroe Carell Jr. Children’s Hospital at Vanderbilt was one of 13 sites participating in the study and the second largest enroller.
“We think that this new lipid formulation can prevent the development of parenteral nutrition-associated liver disease,” said Jörn-Hendrik Weitkamp, M.D., the principal investigator of the local study and an associate professor of pediatrics at Vanderbilt. “SMOFlipid has been used for many years in neonatal units in Europe, and in the United States it is approved by the FDA for use in adults. Our goal now is to get FDA approval for use in infants.”
“SMOFlipid has been used for many years in neonatal units in Europe, and in the United States it is approved by the FDA for use in adults. Our goal now is to get FDA approval for use in infants.”
SMOFlipid
Most conventional lipid emulsions, like Intralipid®, are based on soybean oil, which is rich in omega-6 polyunsaturated fatty acids. In contrast, SMOFlipid contains an almost equal mixture of soybean oil as well as medium-chain triglycerides, olive oil and fish oil.
“One of the biggest differences between the two is that SMOFlipid contains fish oil, which is a rich source of omega-3 fatty acids,” Weitkamp explained. Omega-3 fatty acids have anti-inflammatory properties, and studies suggest that a higher omega-3 to omega-6 fatty acid ratio may prevent liver injury. “The idea is that you decrease inflammation by having more omega-3s,” Weitkamp said.
The Phase 3 Trial
A total of 204 patients enrolled in the double-blinded, controlled trial. The inclusion criteria included neonates and infants expected to require parenteral nutrition for 28 days. Participants received parenteral nutrition with either SMOFlipid or Intralipid®, and the primary outcome measure was the number of patients in each treatment group with conjugated bilirubin levels greater than 2 mg/dL during the first 28 days of study treatment.
Although a final data analysis is pending, enrollment has ended and the FDA will finalize the study with the current number of patients. “Even though it’s not yet formally FDA approved for babies, because our experience has been positive, and based on what other centers are doing in the U.S. and outside the U.S., we are now giving SMOFlipid as a standard of care,” Weitkamp said.
Pushing Forward
Weitkamp is optimistic that the FDA may take into consideration results from studies of SMOFlipid conducted in Europe, as well as the unique challenges of this clinical trial, and continue processing the approval.
“A majority of drugs that we use are not FDA approved for the population. It just doesn’t feel as good as having something that’s actually labeled for the indication.”
However, treating off label is not uncommon in neonatology. “A majority of drugs that we use are not FDA approved for the population. It just doesn’t feel as good as having something that’s actually labeled for the indication,” Weitkamp said. He says that this clinical trial is one example of how large neonatal ICU clinical research programs like Vanderbilt’s can contribute to getting more drugs FDA approved for use in infants.