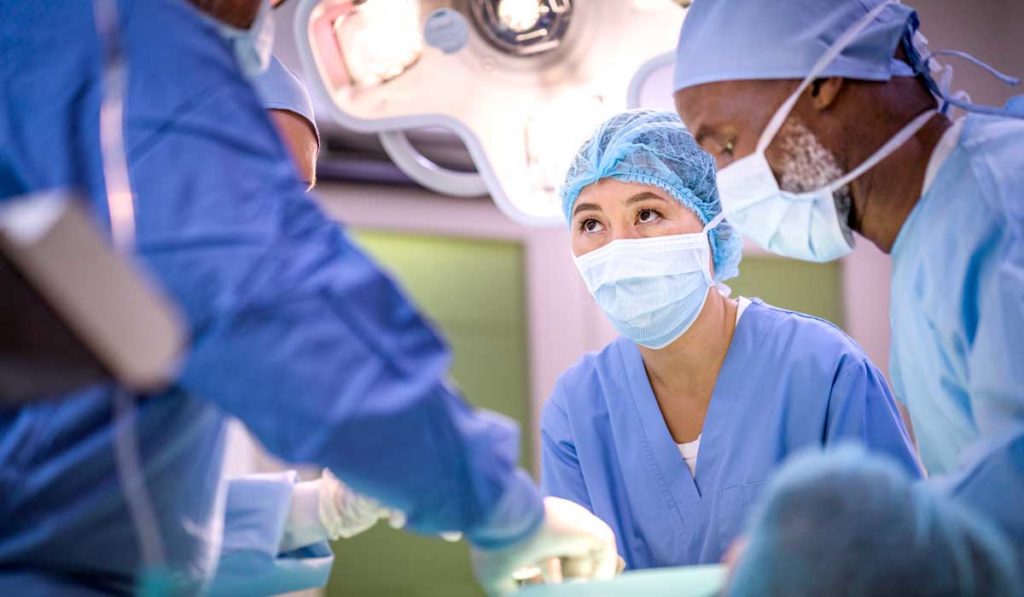
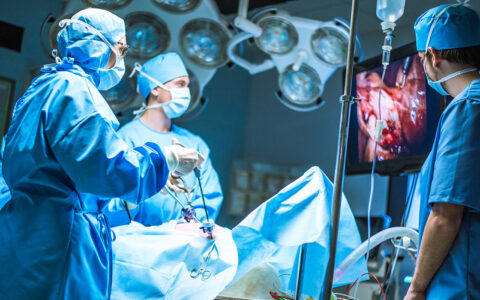
At the beginning of the U.S. COVID-19 outbreak, surgeons at Monroe Carell Jr. Children’s Hospital at Vanderbilt formed a task force to plan the reorganization of perioperative services in response to the virus. Jeffrey Upperman, M.D., Surgeon-in-Chief and an expert in pediatric trauma and disaster preparedness, says from the onset the team heard his call to adopt a long-term view of the pandemic’s impact, and to embrace a spirit of innovation.
“I recognized very quickly that it was going to take months, if not years, to resolve the issues,” Upperman said.
To help in planning, Upperman looked to colleague Jay Wellons, M.D., chief of the Division of Pediatric Neurosurgery at Children’s Hospital. Wellons quickly partnered with colleagues in local anesthesia, surgery and nursing to parse through the massive amounts of early data.
“It became clear early on that even though this was a disease that disproportionately affected adults, children could be asymptomatic carriers,” said Wellons. “We needed to develop ways to protect our health care workers that would reduce the chance of exposure and allow us to keep caring for the children.”
Innovation Under a Crisis
Early in the U.S. pandemic, Wellons joined a national conference led by the team at Seattle Children’s Hospital. The call led to a rapid collaboration with other pediatric surgery leaders nationally on guidelines for perioperative services. Wellons and a group of neurosurgery leaders published the guidelines in JNS Pediatrics.
At Children’s Hospital, they adopted new team structures designed to facilitate agile planning, data-based analysis and lowering barriers to innovation. The new system enabled rapid responses to the task force’s recommendations, explained Barbara Shultz, MSN, R.N., administrative director of Surgical Services.
While priority one was assessment and reallocation of resources, including the labor pool, new daily huddles with hospital leadership and experts across departments allowed the team to continually evaluate data and reprioritize, Shultz said.
Additionally, the team committed to not only share critical information with frontline team members, but to encourage idea generation from the bottom up. In a video interview, Upperman recently described this new culture of open communication and innovation.
“Of course, we have a command and control system but in reality, teams are going to be facing crises upfront in the moment.”
“Of course, we have a command and control system but in reality, teams are going to be facing crises upfront in the moment. I did not want them paralyzed wondering what they thought somebody else needed to do. I wanted them to have trust so that they were not going to fear failing,” Upperman said.
Preserving New Ways of Working
As Tennessee and Nashville follow the national path and open doors to more elective surgeries, other colleagues at Children’s Hospital, including Christopher Wootten, M.D., Director of the Pediatric Otolaryngology Service, are helping to pivot the task force to evaluating reentry from a strategic perspective.
“Some changes will be permanent,” said Wellons. “For instance, long-term strategies are in development for telehealth and other pediatric surgical follow-up protocols.”
All on the task force say they hope to carry forward the environment that prioritizes open communication and collaborating to resolve problems. “We’re all very facile with the language now; there’s been a lot of trust built. If there is a legitimate question, there’s an effort to get an answer. It really underscores the value of transparency.”
Said Upperman, “In this next stage of the pandemic, and what I mean is the next year or two, we’re going to continue to adapt.”