Acute risks of unplanned extubation (UE) are well-documented, but a recent study is one of the first to specifically measure its longer-term effects in preterm infants.
In a Pediatrics study, researchers retrospectively analyzed outcomes, resource use and financial costs of UE in very-low-birthweight infants admitted to level 4, regional neonatal ICU (NICU) at Vanderbilt University Medical Center.
“While our findings were congruent with the adult and pediatric intensive care unit populations, we discovered preterm infant outcomes after UE were worse and the magnitude was more severe,” said first author Leon Dupree Hatch, M.D., a neonatologist at Monroe Carell Jr. Children’s Hospital at Vanderbilt.
Acute Risks
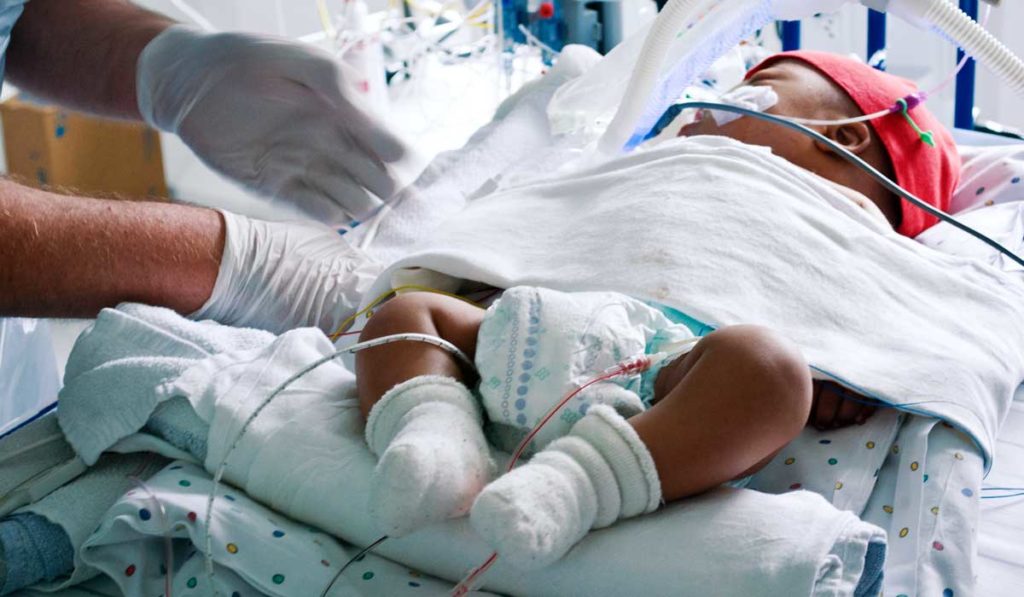
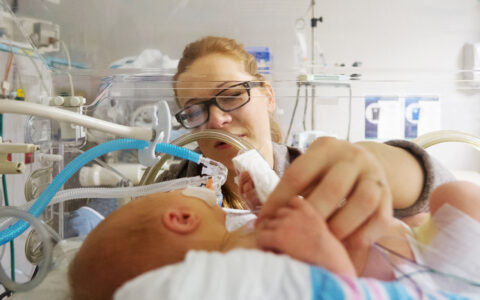
Neonates are at particular risk for UE due to several anatomical and developmental factors, and often require multiple intubations, Hatch said. Oral endotracheal tubes (ETTs) may be removed by the neonate, or by necessity during resuscitation events. They can also become dislodged inadvertently during routine care.
“Short-term patient harm often follows these events, including reintubation, oxygen desaturation, and hemodynamic instability leading to cardiopulmonary resuscitation,” wrote the authors.
“Short-term patient harm often follows these [UE] events.”
Costly Consequences
Dupree and colleagues studied very-low-birth-weight infants (less than 1500 grams) admitted to the NICU within 72 hours of birth without chromosomal or congenital abnormalities, and who received mechanical ventilation through an ETT for at least one hour. The researchers identified UE using four data sources: bedside records, EHR, Vanderbilt’s voluntary incident reporting system, and NICU respiratory therapist records.
The matched cohort study found that across 345 neonates, 58 had at least one UE. Exposure to UE more than doubled post-matching mechanical ventilation days (12.5 days versus 6 days for those without UE). Neonates who experienced UE also spent 10 additional days in the hospital, and incurred a nearly $50,000 increase in total hospital costs.
“Our study was the first to describe what these UEs mean for the baby as well as what impact it has on the NICU,” Hatch said. “The findings are helpful for those working to lower rates of UEs and give us the ammunition to continue to do this important quality improvement work.”
“[The findings] give us the ammunition to continue to do this important quality improvement work.”
Prevention Initiatives
The authors note several national quality improvement efforts are already underway to reduce UE in the NICU. Hatch’s own work has helped identify root causes and gain stakeholder buy-in for such interventions.
Hatch has shown simple NICU workflow adjustments, such as implementing a standardized checklist for intubation, can reduce intubation-associated adverse events by 10 percent. His team is currently looking at the effect of UE on neurodevelopmental outcomes in preterm infants.
“Spending money on prevention will help save lives and costs. If teams have more resources to deal with unplanned extubations, they can not only improve patient care but save money,” he said.