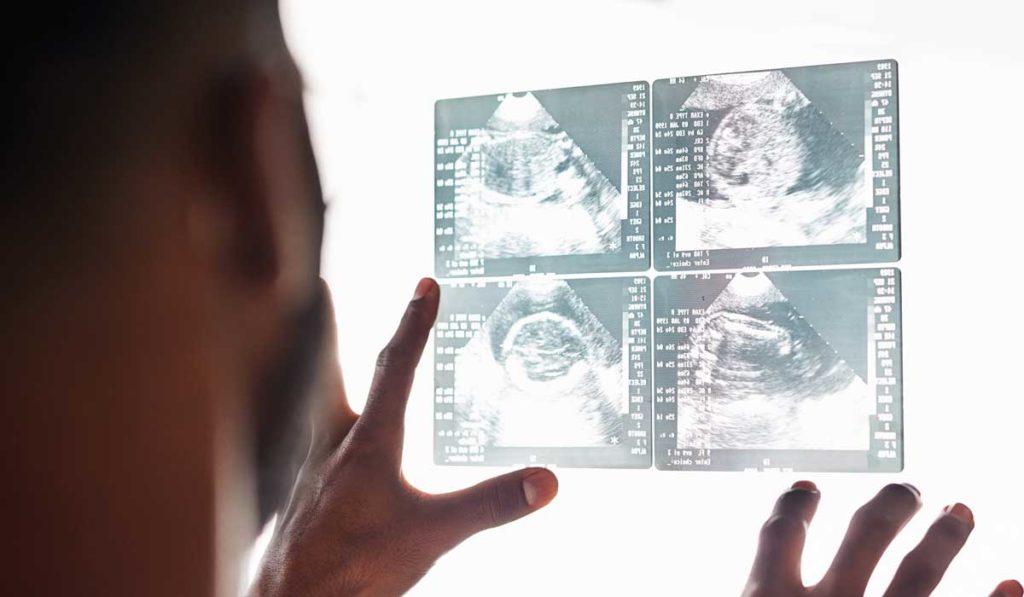
A nine-day program to train head and neck surgeons in Kenya with no prior hands-on experience using ultrasound (US) was effective in conveying clinically valuable skills and knowledge, according to a recent study conducted by faculty and residents from Vanderbilt University Medical Center.
“Outside of seeing pictures of ultrasound equipment in books, every one of the eight trainees had never seen or handled ultrasound equipment. They had had no exposure to ultrasound at all,” said C. Burton Wood, M.D., an otolaryngology resident at Vanderbilt.
The US training took place concurrently with a two-week training camp on head and neck surgery skills. Results were published in The Journal of Surgical Education, authored by Wood and others including Jamie Wiggleton, a nurse practitioner at Vanderbilt, and James Netterville, M.D., associate director of the Bill Wilkerson Center for Otolaryngology and Communications Sciences.
“Outside of seeing pictures of ultrasound equipment in books, every one of the eight trainees had never seen or handled ultrasound equipment. They had had no exposure to ultrasound at all.”
Advantages of Ultrasound
Radiologic imaging is in short supply in low- and middle-income countries (LMICs), where health care organizations cannot afford the high cost to buy and maintain CT scan and MRI devices, Wood says. US technology is more affordable and offers other advantages. It costs relatively little to maintain, requires minimal time to obtain images and involves no side effects.
Nonetheless, in LMICs, US use is often limited to trauma exams, obstetric evaluations, and the evaluation of other uterine or abdominal conditions.
Strong Interest and Investment
“This was a feasibility study, designed to answer three questions,” Wood explained. The research questions addressed participants’ level of interest in the training, the ability to access the needed US technology, and the effectiveness of instruction within the rapid timeframe.
Largely, surgeons from the larger training camp did want to learn to use the US. Eight (62 percent) of 13 African surgeons decided to participate in the US training course. Six were from Kenya, one from Oman and one from Uganda.
Regarding technology availability, the participants had access to a machine in their outpatient areas, but they had not used it previously due to a lack of experience or training. They were working toward raising funds to purchase a more portable system, similar to the two units used in the training course.
“We could donate the device outright, but historically if their hospital system participates, even partially, in the funding of the equipment, then it will be protected and cared for better over time,” Netterville explained.
Improved Assessment of Anatomy
The US training course consisted of five separate lectures focused on head and neck US, given concurrently with interactive US sessions. The researchers found that the rapid training did effectively improve the ability to perform US exams and interpret images.
Participants underwent evaluations of their skills before and after training. Most items in the evaluation gauged proficiency in the assessment of normal anatomic head and neck structures. With the highest score possible being 45, the mean pre-course score was 25 (range 21-30), and the mean post-course score was 40 (range 35-45). Participants of all levels (residents and attending physicians) significantly improved their scores, with an overall mean improvement of 16 points (range 10-23).
“Very few medical outreach trips generate this kind of data,” Netterville said.
Sustaining the Effort
The training camp, held at Tawiq Hospital in Malindi, Kenya, numbers among dozens of surgical education trips in which Vanderbilt head and neck surgeons have participated since 1999. Over time, the focus of these trips has shifted from simply providing patient care to making a difference that sustains and multiplies itself through training.
“Our goal now is to teach surgeons who become teachers themselves.”
“When you go overseas and do head and neck surgery, you leave behind happy patients and happy families and a rural community that feels supported, but as far as sustainable medical outreach, you’ve accomplished nothing,” Netterville said. “Our goal now is to teach surgeons who become teachers themselves.”