Search Results
vads

Helping Children with VADs Live Outside the ICU
ACTION collaborators aim to de-escalate care as patients await transplant.

Taking “Failure” Out of Heart Failure: The Next 10 Years
ACC.19 conference keynote speaker assesses evolution in cardiomyopathy treatment.
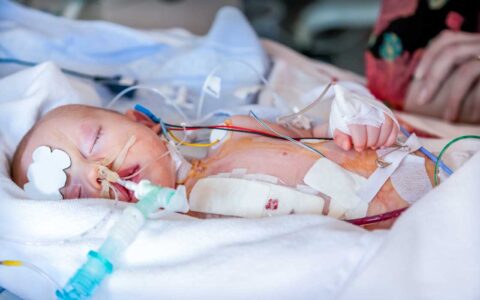
Pediatric and Adult Heart Transplants Surpass Records
Vanderbilt becomes world leader in heart transplantation.

David W. Bearl, M.D.
…Monroe Carell Jr. Children’s Hospital at Vanderbilt. His research focuses on improving outcomes for children awaiting heart transplant, especially those waiting with VADs, and post-transplant outcomes when bridged with VAD….
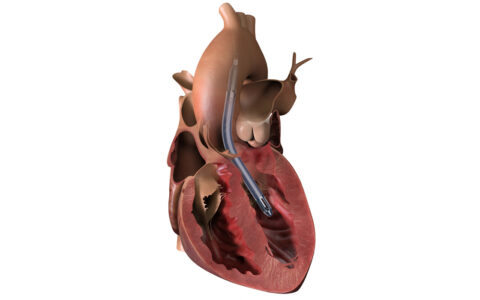
Niche Role for New Miniature VAD
Percutaneous Impella implantation introduced for eligible pediatric patients in select centers.