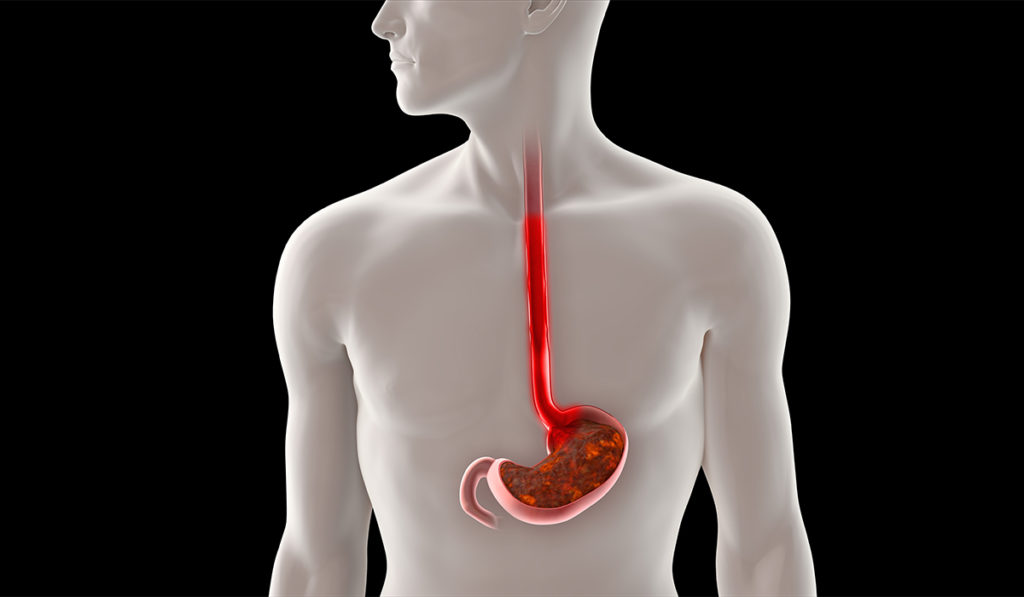
An investigational drug that binds to bile in the stomach may provide relief for patients with difficult-to-treat cases of gastroesophageal reflux (GERD). The drug acts differently from protein-pump inhibitors (PPIs), which are the mainstay of GERD therapy today. PPIs inhibit the harmful effects of digestive acids, but do not inhibit the effects of bile.
The promising findings emerged in a study in Gastroenterology led by Michael F. Vaezi, M.D., director of the Center for Swallowing and Esophageal Disorders at Vanderbilt University Medical Center. Vaezi’s earlier research has shown that the more severe the case of GERD, the more likely it is that bile reflux is a major contributor.
“PPIs are really good at suppressing acid reflux but don’t do much to address bile reflux. This drug offers us a novel way of treating patients with refractory GERD, not just to keep going with more and more acid suppression but to intervene through bile suppression,” Vaezi said.
“This drug offers us a novel way of treating patients with refractory GERD, not just to keep going with more and more acid suppression but to intervene through bile suppression.”
An Alternative Treatment Approach
PPIs, most of which are FDA-approved for once-a-day dosing, work by impeding stomach enzymes with major roles in acid secretion. However, approximately 30 percent of GERD patients remain symptomatic despite the use of once-a-day PPI therapy. Vaezi says this often prompts clinicians to try off-label twice-daily dosing of the PPI or adding another sort of reflux medicine, such as an H2 receptor antagonist.
“These add-on agents are only targeting acid suppression, and not addressing the problem with bile reflux,” Vaezi said.
Vaezi’s new study evaluated the safety and efficacy of three different doses of a medication called IW-3718 as an adjunct therapy to PPIs in patients who either failed to respond to PPI treatment or had only a partial response. Vanderbilt was one of 62 U.S. sites that gathered data on a total of 280 patients with refractory GERD between March 2016 and April 2017.
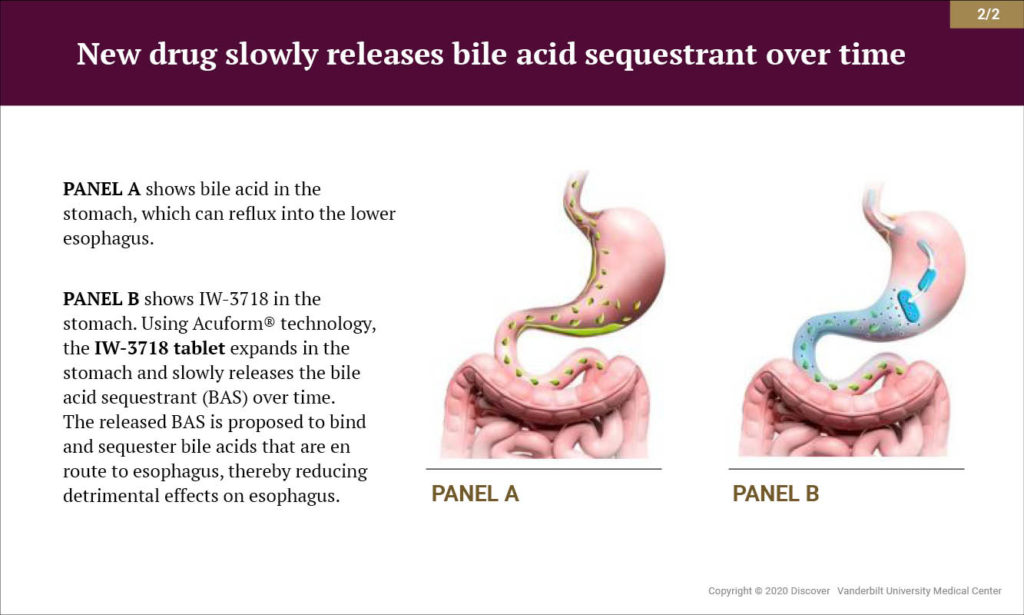
The drug is a special, extended-release formulation taken as a tablet. “It sits in the stomach and slowly releases a bile sequestrant, thus making the bile much less available to reflux into the esophagus,” Vaezi explained.
Promising Results
Patients were randomized to receive placebo or IW-3718 twice daily (500 mg, 1000 mg, or 1500 mg). All patients continued to take their once-daily PPI along with the study-provided medication (or placebo) for eight weeks. The primary endpoint was the percent change in a weekly heartburn severity score, with a secondary endpoint being the percent change in the patient’s weekly regurgitation score. The researchers observed a dose-response trend across treatment groups. Weekly heartburn severity scores were reduced by 58 percent in the 1500 mg treatment group. Patients in the two groups taking lower doses of the IW-3718 experienced intermediate heartburn improvements (55 percent in the 1000 mg group and 49 percent change in the 500 mg group), as compared to 46 percent in the placebo group.
Among patients who experienced regurgitation at baseline, forty-six percent of patients taking 1500 mg of the investigational drug responded with improvements, while 34 percent of the patients on the placebo improved with regard to regurgitation frequency.
“Our results are positive. They confirmed our hypothesis, that this novel way of treating patients with refractory GERD through bile sequestration would make them feel better.”
“Our results are positive. They confirmed our hypothesis, that this novel way of treating patients with refractory GERD through bile sequestration would make them feel better,” Vaezi said.
Chronic GERD: Widespread and Dangerous
With no drug-related serious adverse events in the new study, IW-3718 appears promising to treat a major patient population. About 20 percent of U.S. adults report having GERD-related symptoms weekly and many report having them daily. Symptoms include burning sensations or pain in the chest, problems swallowing, and the regurgitation of food or sour liquid.
Chronic GERD can contribute to problems that include chronic cough, laryngitis, and esophageal inflammation and ulcers. Chronic GERD is also a precursor to Barrett’s esophagus, a condition that raises the risk of esophageal cancer. “With treatments that may allow us to intervene sooner and more effectively to reduce the severity of reflux, we can reduce the likelihood of that progression,” Vaezi said.