Substantial data from a decade of follow-up from the Management of Myelomeningocele Study (MOMS) support that there are a number of significant physical and emotional benefits of fetal myelomeningocele repair.
“Long-term neurological benefits of prenatal surgery include improved mobility and independent functioning and fewer surgeries for shunt placement and revision,” said John W. Brock III, M.D., Monroe Carell Jr. Professor and senior vice president of pediatric surgical services at Vanderbilt University Medical Center.
With respect to urological functioning, however, previous retrospective analyses have not shown conclusively that prenatal repair provided short- or long-term improvements. To dig deeper into the reason, Brock led researchers from Vanderbilt and members of the MOMS Trial Group in a study of urological outcomes in school-age MOMS patients.
The results, published in the Journal of Urology, indicate that fetal repair may improve certain aspects of bladder function when compared with conventional repair.
A Closer Look at Urological Function
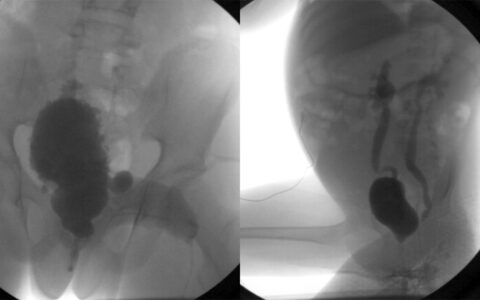
Women who participated in the original MOMS trial were asked for consent to follow-up with their child age six years or older. Participating children underwent urological and radiological procedures at a MOMS center to evaluate current bladder functioning. Primary urological outcome was defined as any of the following: the need for clean intermittent catheterization, vesicostomy, urethral dilatation or augmentation cystoplasty.
The study found that 62 percent in the prenatal surgery group and 87 percent in the postnatal group were placed on clean intermittent catheterization. Twenty-four percent in the prenatal group compared with 4 percent in the postnatal group were reported to be voiding volitionally. Augmentation cystoplasty, vesicostomy and urethral dilation did not differ between the two groups.
“It is unclear why children with prenatal closure of myelomeningocele had less reported clean intermittent catheterization,” Brock said. “Although most children are in diapers or on clean intermittent catheterization, parental reports showed children who underwent prenatal closure may be more likely to void volitionally than the postnatal group.”
Next Steps for MOMS
Fetal surgery to repair spina bifida was pioneered at Vanderbilt University Medical Center in 1997. The earlier MOMS study was conducted from 2003 to 2010, when the NIH ended the trial early after 183 surgeries based on clear evidence that the prenatal surgery was effective, Brock said. In total, 161 of these patients participated in the MOMS2 follow-up.
“That’s the uniqueness of this study — the mere fact that we’ve been able to do it for so long.”
“This is a really unique cohort of patients. We have followed these children and mothers for 17 years, which has allowed us to capture additional data and insight into not only the world of a child born with spina bifida but whether fetal intervention has improved their quality of life,” Brock said. “That’s the uniqueness of this study — the mere fact that we’ve been able to do it for so long.”
MOMS researchers plan to continue to follow the group of children, though specific plans have not been announced. Other Vanderbilt investigators contributing are Timothy Cooper, M.D., an assistant professor of psychology, and Sumit Pruthi, M.D., an associate professor of radiology and radiological sciences.