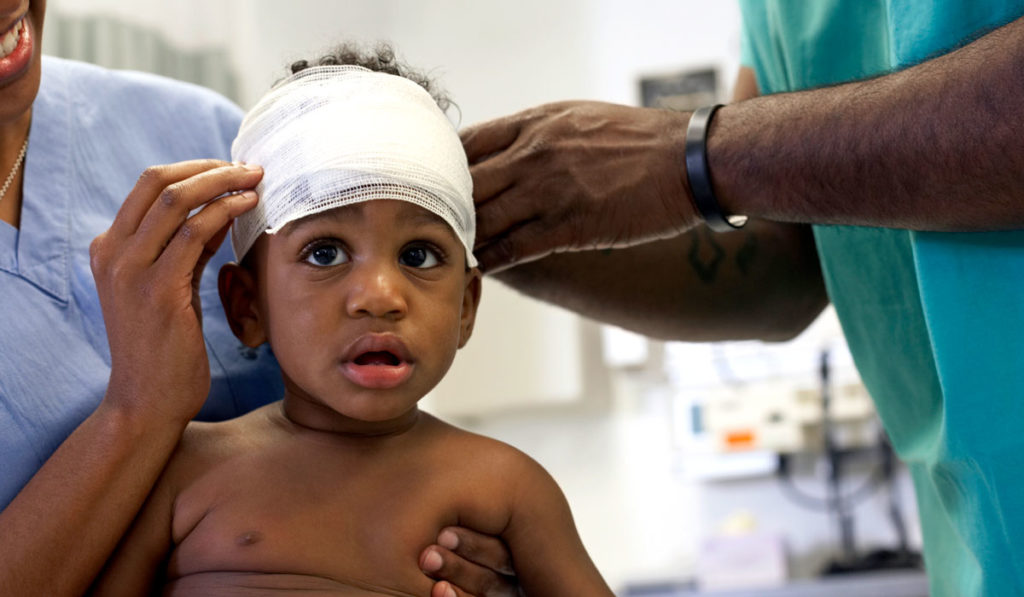
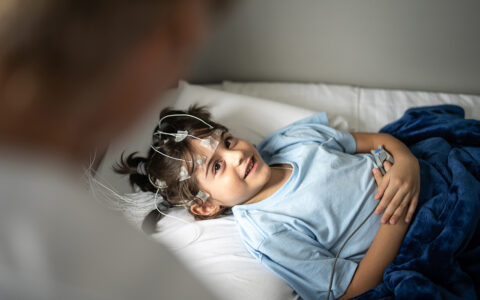
A 12-year retrospective study of pediatric neurosurgical operations for central nervous system (CNS) tumors revealed uniformity in treatment and survival outcomes between self-identifying Caucasian and African American patients, but a marked disparity in missed core follow-up appointments.
This study is part of a larger initiative by the Surgical Outcomes Center for Kids (SOCKs) at Monroe Carell Jr. Children’s Hospital at Vanderbilt to identify and address racial and socioeconomic disparities in pediatric patients undergoing operative treatment.
The findings in CNS tumor patients suggest a pattern that may impact outcomes for other conditions, said senior investigator Jay Wellons, M.D., chief of the Division of Pediatric Neurosurgery at Children’s Hospital. “Together, we hope these types of studies will lead to timely interventions for a greater number of children and more effective use of health care dollars.”
Equal Health Outcomes, Unequal Follow-up
Researchers reviewed data on 198 pediatric patients initially treated for a primary CNS tumor at Children’s Hospital, looking at disparities in initial and follow-up care as well as survival between African-American and Caucasian patients. Primary outcomes included time from symptom presentation to initial neurosurgical consultation and percentage of missed follow-up visits for ancillary or core services.
No significant difference was found in the median time (30 days) from symptom onset to initial presentation. Moreover, no difference was found in survival or other health outcomes.
Marked differences were found in core follow-up visit adherence. African American families missed a median of 11.76 percent of appointments, compared with 3.25 percent among Caucasian patients. There was a significant correlation between insurance status and missed core visits, but no significant associations between missed visits and ethnicity, sex, median income or distance to the treatment center.
“We want to paint a broad picture of how to engage families across each of these conditions, whether symptoms are more insidious or more acute in their presentation, and then look specifically at how to make an impact.”
Variation by Condition
The findings present an interesting comparison with Wellons’ earlier research on race and craniosynostosis (skull shape abnormalities). With craniosynostosis, the disparity manifested as a delay in time to presentation among African American infants. Once care began, time to surgical intervention and follow-up were similar.
“Health care disparity is different depending on the disease. With a brain tumor, the symptoms are acute. Parents get their children to a doctor’s office or to the ER,” Wellons said. “With craniosynostosis, the changes seen in skull growth are slower, less obvious early on.”
Developing customized strategies to improve care based on the disease process is a key focus of SOCKs. “We want to paint a broad picture of how to engage families across each of these conditions, whether symptoms are more insidious or more acute in their presentation, and then look specifically at how to make an impact,” Wellons said.
Improving Outreach
Both studies are helping advance SOCKs efforts to improve follow-up care and family engagement, Wellons explains.
“One of our goals is to identify the most concerning symptoms to focus on in educating parents and referring pediatricians, who are seeing all sorts of things on the ‘front line’ like headaches in the morning, right lower quadrant pain, recurrent urinary tract infections, head growth of an abnormal size, or asthma symptoms that could be gastrointestinal reflux.”
To better connect families to follow-up care, Wellons envisions more use of smartphones and social media. “Particularly for parents who can’t readily get to the pediatrician’s office, we may need to reach them first through social media.” He envisions using social media long-term “as a tool to educate patients, reduce disparity in health care access and improve care.”