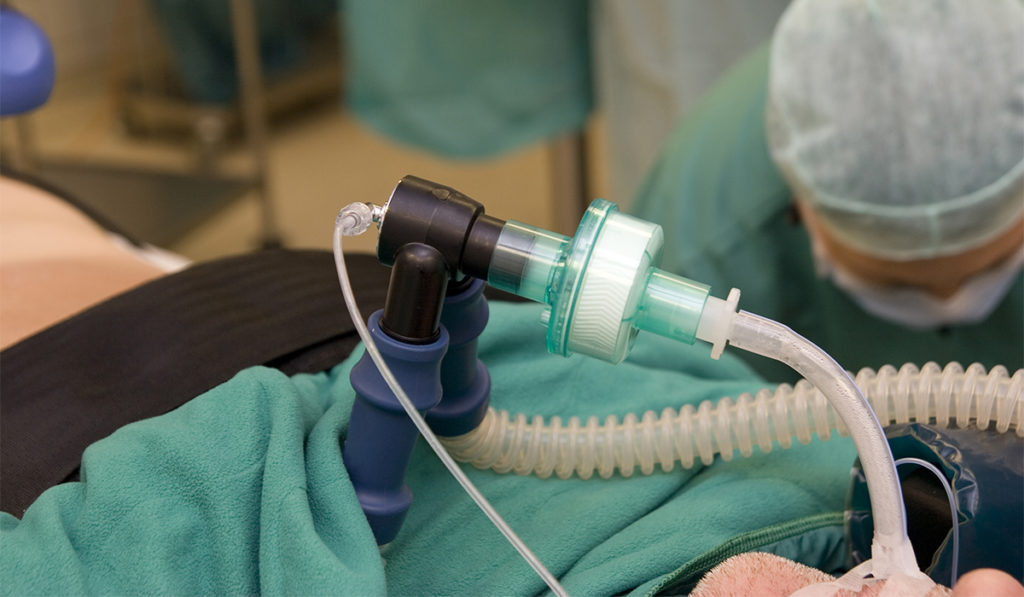
In 2018, Alexander Gelbard, M.D., an otolaryngologist at Vanderbilt University Medical Center, approached Jonathan Casey, M.D., a Vanderbilt critical care physician, to discuss laryngeal injuries he sees in patients who required prolonged endotracheal intubation.
The hallway conversation set into motion a collaborative effort to uncover the causes and scope of these injuries, and how to prevent them. “We view the world from two different perspectives as otolaryngologists and critical care physicians,” Gelbard said. “We set out to establish some clarity and common ground about the impact of intubation on the larynx.”
“We view the world from two different perspectives as otolaryngologists and critical care physicians. We set out to establish some clarity and common ground.”
“As intensivists, our focus is an acute life-threatening illness, and we do not have the opportunity to see long-term complications of tracheal intubation which present months later in the outpatient setting,” Casey said.
To investigate the association between what Casey sees in ICU and what Gelbard sees in the clinic, the team examined 100 consecutive patients who were intubated for over 12 hours. They performed laryngeal endoscopy within 36 hours post-extubation looking for two common types of intubation-related injury: mucosal ulceration or granulation tissue in the larynx that they have named acute laryngeal injury (ALgI) and unilateral vocal fold immobility (UVFI).
Post-extubation Ulceration is Widespread
In their first study, published in Critical Care Medicine, the team found that ALgI (which Gelbard equates to a pressure ulcer of the larynx) occurred with startling frequency. The team found ALgI in 57 out of the 100 patients. Ten weeks later, patients with ALgI reported worse breathing and voice outcomes than those who had not experienced a laryngeal injury.
The findings do not surprise Gelbard, whose clinical practice is focused on patients with severe scarring in the larynx and trachea. “Airway injuries have a tremendous impact on patients after critical illness. Even after they survived their life-threatening illness, they may feel like they are breathing through a small straw.” Analysis of potential risk factors suggested that diabetes mellitus, a high BMI and large endotracheal tubes (ETTs) put patients at higher risk of ulceration, supporting Gelbard’s suspicion that ALgI represents a pressure ulcer in the airway.
Distinct Causes
Their second study in JAMA Otolaryngology-Head and Neck Surgery revealed that seven of the 100 patients developed UVFI. Surprisingly, the patients and risk factors were completely different from those who experienced ALgI. In these seven patients, poor vascular health was the common denominator – all were hypotensive and on vasopressors while intubated. Pre-admission peripheral vascular disease or coronary artery disease were additional risk factors for developing UVFI.
Six of the seven patients had left-side paralysis, which Gelbard says may be associated with the longer course of the left recurrent laryngeal nerve, rendering it more susceptible to perfusion injury. “The evidence points to nerve ischemia as the result of poor tissue perfusion in these patients,” Gelbard says. Unlike ALgI, ETT size was not associated with UVFI.
Testing Preventive Interventions
Gelbard and Casey have devised a three-pronged approach to researching interventions to prevent vocal cord injury. In one study, Gelbard is conducting a clinical trial testing oral antibiotics and a steroid inhaler as a means of reducing the impact of ALgI.
The team is also developing a trial to test whether smaller ETTs can reduce ALgI incidence. Casey says large tubes are used because they allow easier clearance of secretions and easier access for endoscopic procedures in the lungs. “But the truth is we rarely do endoscopic procedures in these patients and smaller tubes may be sufficient for secretion clearance. We need to reassess the risk/benefit equation,” he said.
“The truth is we rarely do endoscopic procedures in these patients and smaller tubes may be sufficient for secretion clearance. We need to reassess the risk/benefit equation.”
Their third step will be to develop protocols for systematically identifying patients who are at high risk for injury and performing bedside examinations soon after extubation.