When it comes to gun violence, many U.S. physicians have found themselves inadvertently as policy advocates. Health care systems are on the front line and bear a major financial burden to treat firearm injuries: some annual cost estimates top $48 billion.
Calls to action are bolstered by mounds of state and national data highlighting grand totals. “But to really understand the problem, you need to look at granular, site-specific data,” said Jeff Martus, M.D., a pediatric orthopaedic surgeon at Monroe Carell Children’s Hospital at Vanderbilt.
Cost Analysis
Martus, together with Vanderbilt pediatric surgeon Harold “Bo” Lovvorn, M.D. and general surgery resident Parker Evans, M.D., recently analyzed pediatric musculoskeletal firearm injuries treated at Vanderbilt’s level 1 trauma center over a 14-year period. The research team mined retrospective, detailed data to characterize the injuries and their financial impact.
Results reported in the Journal of Pediatric Surgery describe 142 distinct orthopedic injuries with total adjusted charges of $11.4 million. The majority of injuries (59 percent) were the result of a violent assault.
Most patients were admitted (73 percent, median LOS 2 days), plus 43 percent later required additional costly hospitalizations, ED visits, or outpatient surgeries. Costs to the hospital totaled $3.7 million and net revenues were $45,042 over the 14-year time period. Secondary hospitalizations incurred a negative net revenue of -$11,225. Said Martus, “Total hospital costs of these injuries represent a considerable financial impact, with a virtually negligible total net revenue. Nobody wins here.”
Insurance Ties
Most victims in the study were male (84 percent). Forty-two percent were Caucasian, and 52 percent African American. Sixty-one percent had Medicaid insurance. Only nine percent were uninsured – a remarkably low number, Martus said.
Only patients with private insurance (32 percent) generated positive net revenue. Said Martus, “Centers that treat different patient populations – with fewer patients covered by private insurance and more uninsured patients – likely experience an even greater financial burden related to firearm injuries.”
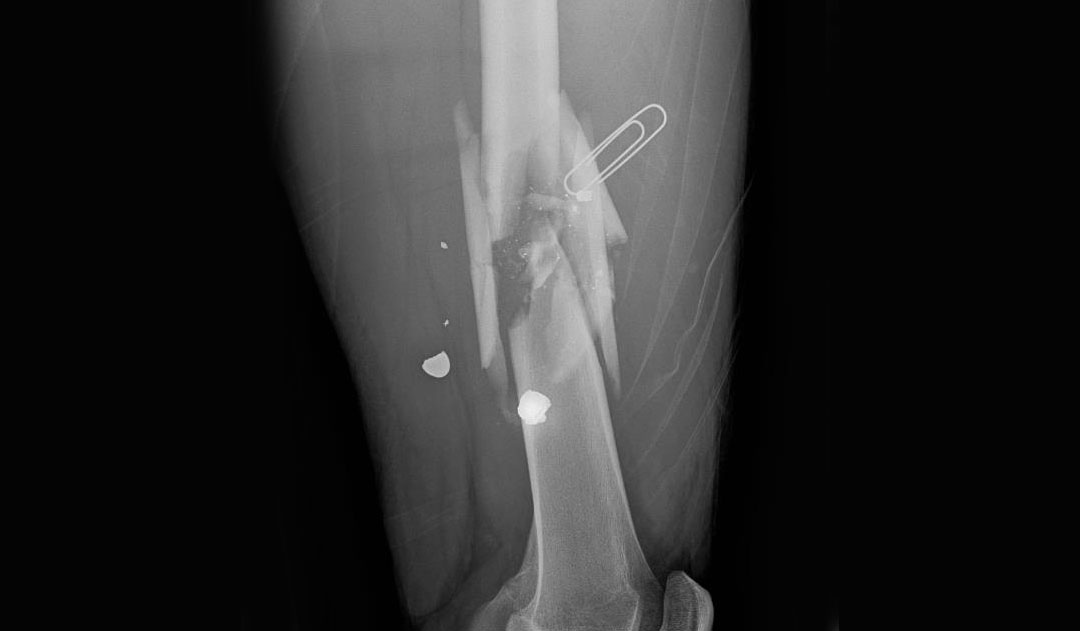
Breadth of Injury
The researchers found a broad range of morbidity underlying the cost of care. For example, one patient with a small pellet gun injury was treated at the bedside and discharged the same day. But another experienced multiple vertebral fractures and paraplegia from a violent shooting. This patient had 96 hospital encounters over the next 3.5 years for a total of 352 admission days – all before being lost to follow up.
Forty-two percent of the patients had at least one complication related to the injury including infection, neurovascular injury, compartment syndrome, and/or spinal cord injury. Seven patients required an amputation (5 percent).
The typical patient fell somewhere between these extremes (though only nine percent of injuries were due to BB/pellet guns). Mixed injury patterns caused by shotguns were the costliest. Said Martus, “Most of the injuries we see are due to shotguns, rifles and handguns.”
“Centers that treat different patient populations – with fewer patients covered by private insurance and more uninsured patients – likely experience an even greater financial burden related to firearm injuries.”
An Opportunity for Action
The study paints a picture of a steady stream of musculoskeletal firearm injuries primarily caused by violence. However, it also provides a deeper understanding of the issue and opportunities for local action.
“Forty percent of the injuries at our center were unintentional,” Martus said. “This is a multifaceted public health issue that demands social improvements, starting with gun safety and education in homes with children.”
Demographic and financial analyses of other firearm injuries (including abdominal, thoracic and cranial injuries) may also reveal intervention opportunities, wrote the authors, noting support for “firearm injury prevention programs that are targeted to at-risk communities, a goal which requires both public support and city-specific knowledge of injury patterns.”






