Vasculitis syndromes, systemic autoimmune diseases that affect blood vessels, sent around 100,000 Americans to the hospital last year. Classified as “rare,” many vasculitis syndromes have never been addressed in formal practice guidelines. To remedy this, the American College of Rheumatology (ACR) assembled a writing group to comb through over 14,000 studies and establish the first evidence-based clinical guidelines for U.S. providers, covering seven vasculitis syndromes.
“These are dangerous diseases that can cause a lot of damage.”
Kevin Byram, M.D., director of the Vanderbilt Vasculitis Clinic, served on the literature review committee for the guidelines, which were presented at the 2019 ACR Annual Meeting and will be published in the next six months. “These are dangerous diseases that can cause a lot of damage. The idea is to provide guidelines to support earlier diagnosis, treatment and limitation of damage,” Byram said.
The timing is apt, with a number of steroid-sparing therapies recently FDA approved. For some forms of vasculitis, the guidelines support the use of new drugs like tocilizumab, mepolizumab and rituximab, all within the biologic medication class, in an attempt to spare glucocorticoids. The guidelines also emphasize imaging advances that are enabling earlier and more localized identification of vessel disease.
Complex Syndromes Call for Nuanced Guidance
The umbrella term “vasculitis” covers a host of syndromes that vary in character, sites affected and severity. “Symptoms can mimic infection, so recognizing the differentiators can be confusing for a primary care provider, or even for a rheumatologist, who may rarely encounter a patient with vasculitis,” Byram said.
Monitoring and adjusting treatment requires a flexible, nuanced approach. “Really, the aim of these guidelines is to help community rheumatologists by giving them a resource – almost an FAQ – on how to manage these complex patients,” he said.
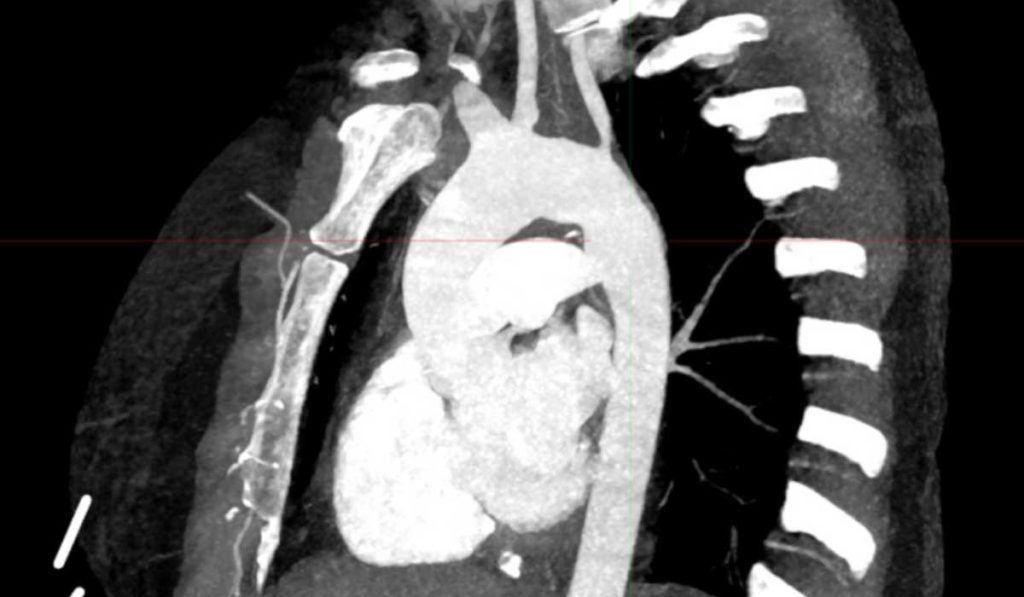
On the diagnostic front, the guidelines suggest a significant role for CT, MRI, and PET scans. “The role of advanced imaging in vasculitis diagnosis has been studied a lot in the last few years. These scans have the capacity to identify and differentiate vasculitis syndromes at a very early stage,” he said.
“These scans have the capacity to identify and differentiate vasculitis syndromes at a very early stage.”
Ultrasound, however, has been given a yellow light. While the European League Against Rheumatism recommends ultrasound over temporal artery biopsy for making a giant cell arteritis diagnosis, Byram and other ACR guideline authors are reticent to agree, citing lack of sufficient experience among U.S. practitioners in using ultrasound for this kind of application.
Role of New Biologics
The guidelines focus largely on drug therapies, recognizing the role biologics play in reducing the side effects of traditional treatments. For treating the most common syndrome, giant cell arteritis, tocilizumab is recommended in conjunction with glucocorticoids. In anti-neutrophil cytoplasmic antibody vasculitis syndromes, rituximab is conditionally favored over cyclophosphamide.
The ACR strongly recommends tumor necrosis factor to treat a newly discovered vasculitis phenotype, DADA2-associated polyarteritis nodosa, based on impressive data that suggest it prevents stroke.
While all immunosuppressive drugs raise infection risks, these substitutes avoid some of corticosteroids’ most notorious side effects, with weight gain and diabetes, cataracts and osteoporosis chief among them.
The guidelines do not directly address non-pharmacologic treatments, but Byram emphasizes the beneficial roles of exercise to enhance blood flow to the limbs in patients with large vessel vasculitis, and pulmonary rehabilitation with patients who have experienced pulmonary sequelae of vasculitis. “In some forms of vasculitis, these go a long distance in minimizing the dosage and frequency of drugs and substantially improving function,” Byram said.