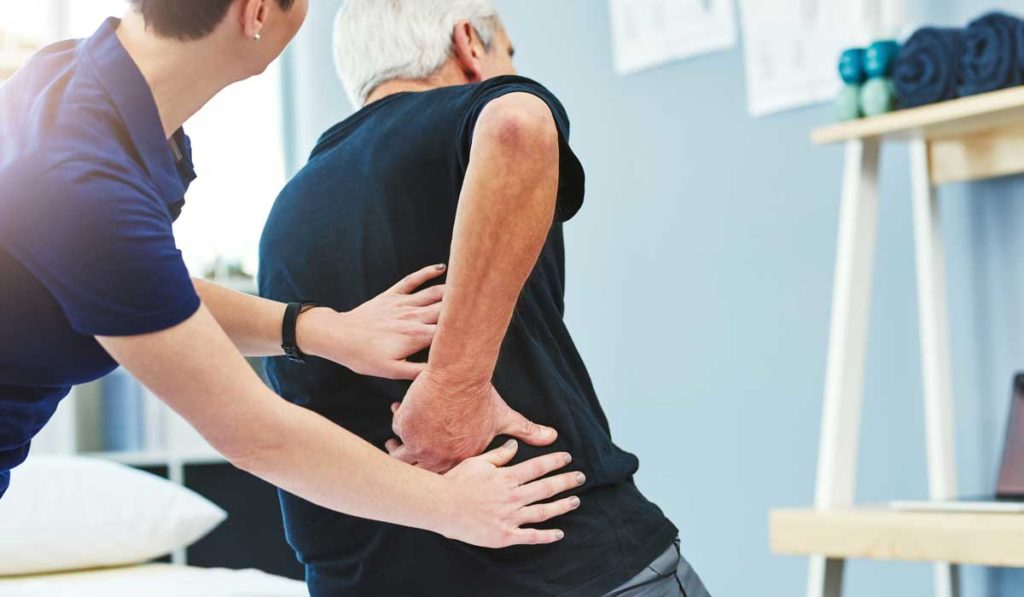
In a recent study published in PLOS ONE, primary care physicians (PCPs) in four cities identified numerous challenges to providing optimal CKD care, including a lack of recognition among patients. Chronic kidney disease (CKD) affects an estimated 15 percent of U.S. adults – 37 million people – but most (9 in 10) are unaware they have it.
“Chronic kidney disease is one of the least understood conditions – by both patients and providers,” said Kerri Cavanaugh, M.D., associate professor of nephrology and hypertension at Vanderbilt University Medical Center. “Our aim was to find out why and to recommend strategies for improvement.”
Cavanaugh and Khaled Abdel-Kader, M.D., assistant professor of nephrology and hypertension at Vanderbilt, were co-authors on the paper, written by the National Kidney Foundation (NKF) Education Committee. The study aligns with the recent White House Executive Order on Advancing American Kidney Health that aims to prevent kidney failure through better diagnosis, treatment, and incentives; increase patient choice by educating them on treatment alternatives, and increase access to kidney transplants.
Patient-level Barriers
Investigators used a mixed-method approach (surveys and 90-minute focus groups) to build on existing evidence and provide detailed views of the challenges U.S. PCPs face in caring for patients with CKD.
Thirty-two community-based PCPs participated in the study. They identified patient-level barriers to be poor awareness and understanding of the condition, and the high burden of health care costs to patients. This concern was further reinforced in patients having to take time off from work to attend visits and lack of knowledge about alternative options, such as home dialysis.
PCPs also described the frustrations they experience in engaging patients in self-management of CKD risk factors. “Although the majority of PCPs reported feeling comfortable educating patients about CKD,” Cavanaugh said, “they felt they had insufficient, readily available resources to improve patients’ understanding of their diagnosis and to support patient self-management.”
“PCPs felt they had insufficient readily available resources to improve patients’ understanding of their diagnosis and to support patient self-management.”
Provider Challenges
PCPs in the study reported they had limited CKD knowledge relative to other diseases and difficulty managing CKD-associated complications (e.g. metabolic acidosis, bone disorders, or anemia) and comorbid illnesses. They also described challenges in recognizing CKD due to the use of creatinine rather than estimated glomerular filtration rate, and the lack of CKD documentation on the EHR problem list.
Forty-five percent of respondents reported not following the NKF Kidney Disease Outcomes Quality Initiative (K/DOQI) guidelines for CKD care. Some had limited familiarity with the guidelines, while others felt the guidelines were for nephrologists and perceived an absence of clear, easily applied algorithms for CKD management.
System-level Barriers
Systems-level barriers to providing CKD treatment included insufficient time for managing complicated disease processes, limited reimbursement, rigid EHR templates, and inadequate clinical and educational resources. PCPs also reported a need for infrastructure resources. They suggested a more robust implementation of value-based care models and patient-centered medical homes, and greater ease in accessing multidisciplinary care teams. Some respondents suggested that reframing expectations in CKD care may be required.
The study concluded that to increase capacity to effectively care for CKD patients and achieve Healthy People 2020 CKD objectives, efforts are needed to improve dissemination of educational tools and patient resources, enhance PCPs’ CKD knowledge and facilitate adherence to guidelines.
“The findings were pretty consistent with the usual conversations in this area,” Cavanaugh said. “Now we have to work toward implementation. The bottom line is that all of us as physicians want better care for our patients with CKD.”