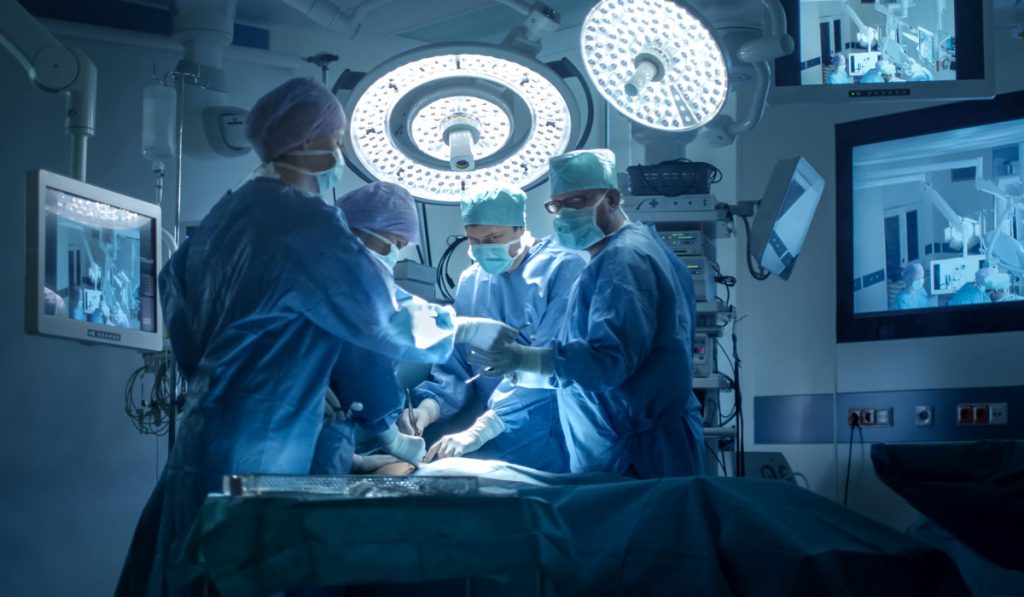
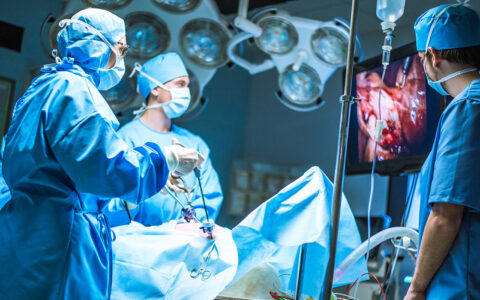
A new era of surgical transparency is emerging, fueled largely by the advent of video recording for quality improvement and the expansion of endoscopic, camera-driven procedures. This push toward more openness in the operating room (OR) is being driven by both patients and the healthcare establishment and is part of the larger conversation surrounding surgical ethics—how surgeons and surgical team members make decisions that result in the highest-quality patient care.
“During surgery, anesthetized patients voluntarily abdicate their active autonomy and can’t participate in moment-to-moment decisions,” said Alexander Langerman, M.D., associate professor of medicine at Vanderbilt University Medical Center and director of the Surgical Ethics Program in the Vanderbilt Center for Biomedical Ethics and Society. “This leaves the surgeon responsible for obtaining informed consent, keeping records of surgeries, identifying performance errors, and determining ways to improve processes. Surgical recording can facilitate this process and alleviate the doubt some patients feel.”
Pros and Cons of OR Transparency
Patient demand for greater transparency may reflect a growing suspicion of authority figures or a fear of not waking up from anesthesia. But patients are also intrigued by what is happening to them while they’re in surgery. Studies suggest that some patients feel less anxious about staying awake during surgery than they do about being sedated. “We are studying both patient perceptions and resident perceptions to understand the effect surgical transparency and awake procedures will have on the surgeon-patient relationship,” Langerman said.
“The OR is a sacred space—it’s our community, our home.”
Despite the clear benefits to understanding and improving their ORs, many surgeons remain resistant to being monitored. “No one wants to fall below the bell curve,” said Langerman. “Plus, the OR is a sacred space—it’s our community, our home.” He believes physicians and healthcare leaders must carefully consider the potential effects that recording can have on both team behavior and patient privacy.
Building an Infrastructure for Research
Vanderbilt’s Surgical Ethics Program provides the collaborative infrastructure for investigations into topics important to surgical patient care such as informed consent, surgical training, overlapping surgery, trauma ethics, error disclosure, and surgical video.
“Our strength is that we’re doing empirical studies on ethics in addition to taking the deep thought, philosophical approach,” Langerman said. “We’re not only collecting data ourselves; we’re focusing on how to enhance the methods that anyone can use for empiric surgical ethics—promoting studies; creating a clearinghouse of surgical ethics papers; assembling resources for investigators. We have a critical mass of highly talented surgeons and colleagues working on ethics scholarship, and this is the right place and time to be taking surgical ethics to the next level.”
Working with Vanderbilt Biomedical Engineering colleagues, Langerman is developing a wearable camera for open surgery as “enabling technology” for surgical scholarship. While most current safety and performance research using surgical video has been limited to endoscopic procedures, this new camera, dubbed Cleopatra, will enable extension of these studies to more common “open” procedures. The camera would enable a video library of open surgical procedures, a long-standing goal of the Vanderbilt Head and Neck Surgery group.
While these cameras would be a boon for patient safety and performance research, they carry with them a host of privacy and data use concerns—a topic Langerman is actively studying in a partnership with the International Center for Surgical Safety, where he serves as an affiliated scientist.
Teaching Surgical Ethics
In addition to research, the Surgical Ethics Program hopes to enhance the quality and impact of surgical ethics in practice and scholarship. Participating faculty provide education; disseminate their knowledge through publications and presentations internationally; and train students, residents and faculty in surgical ethics research.
“A big part of our mission,” Langerman said, “is identifying and developing ethics competencies in surgical trainees. We’re trying to prepare them for a more transparent future.”