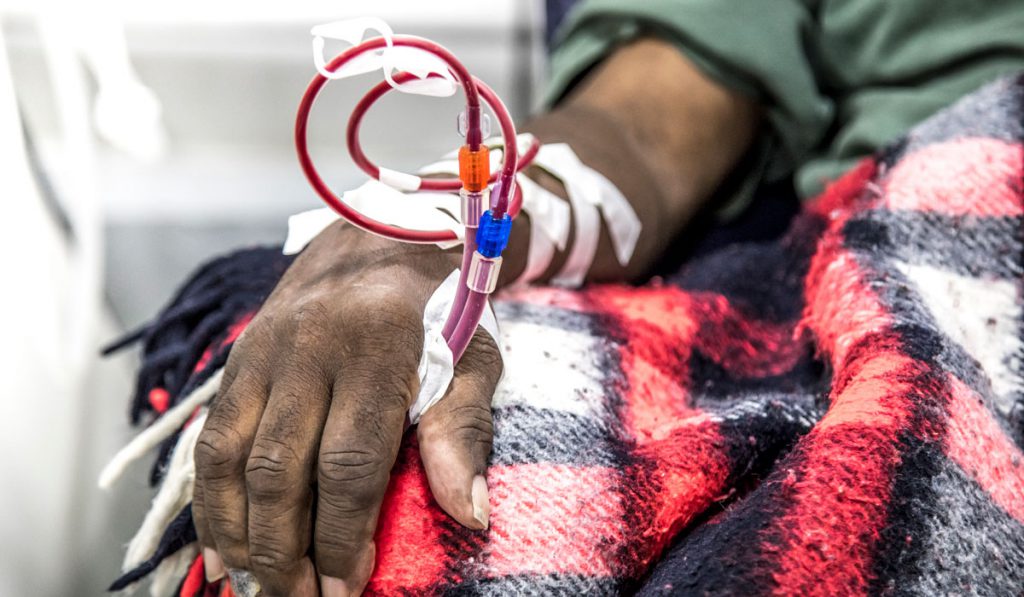
An inadequate national policy toward Medicare reimbursement for home dialysis is one of the longstanding problems hindering expansion of the life-saving treatment, says Thomas Golper, M.D., a professor of nephrology and hypertension at Vanderbilt University Medical Center and national authority in home dialysis programs.
“About 500,000 people in this country are on dialysis,” Golper says. “The most expensive way to treat these patients is to build a building, hire people and do dialysis in that building. Yet that is the system Medicare rewards in most regions.”
“The most expensive way to treat these patients is to build a building, hire people and do dialysis in that building.
Golper, who launched one of the largest home dialysis programs in the country at Vanderbilt, serves 135-150 patients on home dialysis at any given time. He has advocated for changes in Medicare policy to grant home dialysis equal and consistent coverage on a national basis.
Golper is also a dedicated educator, mentor and program builder, who has focused his efforts on encouraging national nursing and physician groups to train home dialysis caregivers, incorporating home dialysis into medical school curricula, and making skilled physicians available to the large dialysis corporations to improve expertise and quality of care.
Barriers to Home Dialysis Availability
In terms of Medicare policy, Golper’s biggest vexation is the fact that the regional Medicare administration contractors (MACs) dictate how home dialysis is covered. “CMS headquarters punted on a national policy for home dialysis reimbursement, citing lack of evidence,” he says. As a result, the 12 regional MACS can have widely varying reimbursement schedules. Texas cut home dialysis benefits in 2017 while Palmetto, Golper’s home MAC for which he serves as Tennessee nephrology representative, offers broad coverage. “There are no regional population differences that indicate it shouldn’t be reimbursed consistently through a nationwide policy.”
A second barrier is a shortsighted focus on the higher cost of more frequent dialysis. While home dialysis averages five to six times per week versus three for institutional hemodialysis, this is far from the whole picture. Hospitalization expenses are lower for home dialysis patients, making total expenses $19,000 less per year on average. Studies show home dialysis patients are more satisfied with their treatment.
The third barrier is one Golper spends extraordinary energy working to break down: the shortage of nurses and physicians who are trained to work with patients on home dialysis. “Doctors won’t refer if they know there is a nursing problem,” Golper says. “Training professionals for home dialysis has not made the priority list for either the American Nephrology Nurses Association (ANNA) or the American Society of Nephrology (ASN), but that battle is far from over.”
Initiatives for Supporting the Home Option
Golper runs a program called Home Dialysis University. It is a three-day course offered five times a year for fellows and practicing physicians. “I train half to two-thirds of all the fellows in the country who learn this,” he says. At one time, nurses were enrolled in a similar program, but participation dwindled. He is entreating ANNA to support a revival. “I have said, you organize the room and the nursing credits and I’ll provide a venue and world class speakers.”
While hospital systems like Vanderbilt often own their home dialysis units, they contract with the large corporate dialysis providers to manage the services. Golper is launching an effort to make trained nephrologists available to consult physician staff at DaVita and Fresensius. “We get calls all the time from their people who have attended our courses, but we want to formalize this.” He plans to follow with nurse-to-nurse mentoring.
Hoping that the key to effecting change in national policy may be more evidence, Golper helped orchestrate a research group, the North American Research Consortium, that is pooling data for research. “We don’t have randomized studies to show that home dialysis outcomes are superior to in-center hemodialysis because you can’t tell patients this sick that they are assigned to this group or that group. They self-select, which degrades the science of the outcomes data.”
“The behavioral evidence is there: 4,000 people in this country are choosing to do this.”
Golper does not, however, intend to await further evidence to recruit and train the next generation of home dialysis caregivers. “If the patients didn’t think it was enough of a benefit, why would they do it? Given a choice between going to a dialysis clinic three times a week and doing it at home five or six, why would you do it more often if it didn’t benefit your lifestyle and help you feel better? The behavioral evidence is there: 4,000 people in this country are choosing to do this.”