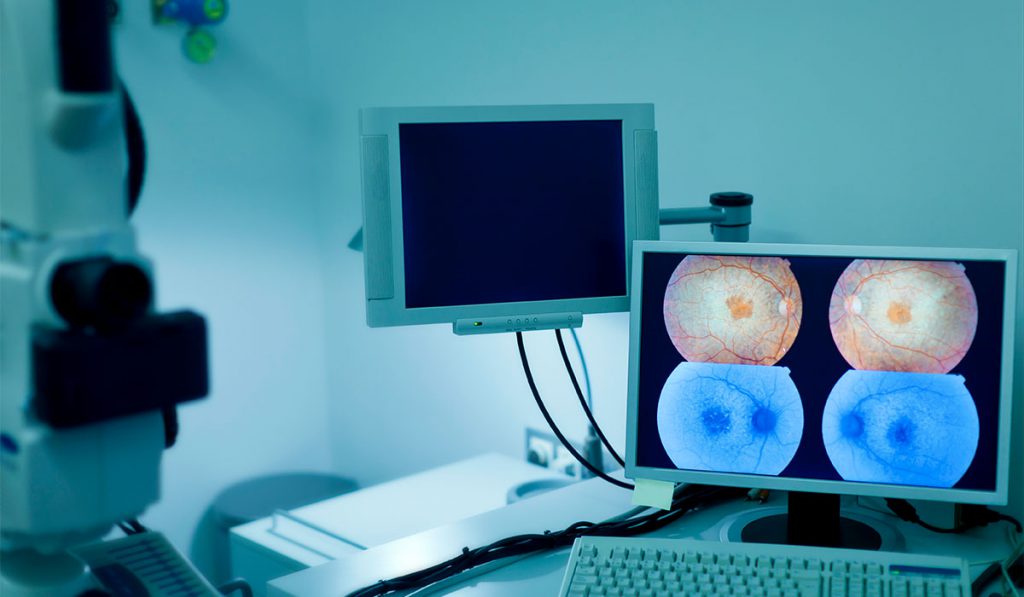
Telemedicine has been used effectively in the diagnosis and monitoring of diabetic retinopathy (DR), the leading cause of blindness among U.S. adults. Yet, the screening rate for DR remains steady at less than 50 percent among diabetic patients in part due to cost, lack of access to eye care providers and poor compliance.
“The current medical paradigm of referring patients into ‘eye care provider networks’ is inadequate for population-based management of diabetic eye disease,” said Edward Chaum, M.D., Margy Ann and J. Donald M. Gass Chair in Ophthalmology at the Vanderbilt Eye Institute. “We continue to have poor visual outcomes because half the patients with diabetes do not receive their recommended annual eye examinations.”
Chaum and other Vanderbilt specialists are working on several projects to expand telemedicine to screen diabetic patients for retinopathy in the primary care setting.
Long-distance Diagnoses
Chaum is a co-developer of a telemedical network and DR screening technology that is now part of the RetinaVue® Care Delivery Model. RetinaVue® provides DR screening in primary care practices (PCPs) and underserved communities in all 50 states and rural Australia.
Low-cost RetinaVue® cameras are distributed to PCPs to conduct the DR screening. The PCP sends the images to a national network of retina specialists via a HIPAA-compliant connection, and the diagnosis is returned with a management plan based on disease severity. The patient with DR is then referred to a retina specialist.
“There are large counties in the U.S. that have very few physicians and almost no specialists,” Chaum said. “This provides for real-time, expert diagnosis and management of diabetic retinopathy in the local community – wherever that community is located.”
Closing the Gap in DR Referrals
The biggest challenge with telemedical DR screening, Chaum explained, is that many patients screened at PCPs do not follow up on the referrals. Additionally, data are limited regarding the clinical outcomes of follow-up treatment because patients are referred for care outside of the PCP network.
“One of the problems with telemedical screening for DR is that it has been an open loop. Primary care practices don’t get any feedback.”
“One of the problems with telemedical screening for DR is that it has been an open loop,” he said. “Primary care practices don’t get any feedback after the patient is sent to a retina specialist.”
In a study to be published later this year, Chaum and colleagues tracked 112 patients diagnosed with DR using telemedicine and requiring treatment by a retina specialist. Fifty percent saw a specialist within six months; after one year, only 75 percent had seen a specialist. At two years, 15 percent of patients still had not followed up on the referral.
Improving DR Outcomes
Locally, the Vanderbilt Eye Institute is working to strengthen DR follow up and outcomes tracking through an integrated referral network. The network includes Vanderbilt adult primary care and endocrinology practices, the Vanderbilt Health Affiliated Network, and the Metropolitan Nashville Public School system’s health plan.
Chaum hopes the network can help close the significant gap in treatment following PCP referrals and be a model for other telemedical screening programs. “We’ll have these patients in our EHR system so we can manage them through the active phase of their disease and demonstrate improved visual outcomes,” he said.
Chaum adds that the COVID-19 pandemic has escalated telemedicine use in ophthalmology. In addition to diagnosis, Vanderbilt ophthalmologists are now using telemedical tools for simple triage, routine post-op care, and plastics and strabismus follow-up.