Physiatrists can put their skills to powerful use when evaluating patients’ pain, says Vartgez Mansourian, M.D., assistant professor of Physical Medicine and Rehabilitation at Vanderbilt Stallworth Rehabilitation Hospital and medical director of Vanderbilt’s Stroke Rehabilitation Program.
Mansourian has received top reviews at Vanderbilt and elsewhere for his unique approach to patients’ whole health. Since joining Vanderbilt in 2016, he has earned patient satisfaction scores in the 98th percentile nationally. Mansourian credits his success with patients to his focus as a physiatrist on looking for underlying conditions potentially overlooked by single-organ specialists, and to his emphasis on treating patients holistically.
“Our background as physiatrists is so unique… we have the ability to both correct the underlying mechanism of dysfunction and provide therapies – exercise, dietary change or medication – to help rehabilitate the patient.”
The Importance of Patient Social History
Gathering all possible information includes taking a thorough social history. For patients who are aphasic due to stroke or who have dementia, this includes speaking with families and caregivers to supplement the patient’s medical record.
“Whenever I get a call that a family member wants to talk, I make myself available,” Mansourian said. “You can develop a trust with family or friends that is critically important, and you may gain information to solve the puzzle of what is happening with the patient.”
Mansourian recalls one patient, an active male in his 70s, who was hospitalized due to sudden changes in mental state, speech, gait and bladder control. The patient was initially diagnosed with normal pressure hydrocephaly (NPH) by attending physicians. Mansourian, however, suspected Wernicke’s encephalopathy (B1, or thiamine, depletion) after asking the patient’s daughter about his social life and drinking habits.
“I ask this question of every patient or family during my system review and social history. In this case, the patient drank an average of six glasses of wine daily,” said Mansourian. After administering intravenous thiamine to the patient, Mansourian saw the patient regain speech within 24 hours and full baseline function within several days.
Evaluation: Considering Alternative Diagnoses
Evaluation is an opportunity to consider alternative diagnoses. “As physiatrists, we’re trained extensively in musculoskeletal evaluations, so we can and must use those skills to verify patient reports,” Mansourian said. “Things can be missed.”
One former patient, a woman in her 70s, presented to Rehabilitation with recurring pain in her lower back and left knee. She had received ESIs from a spine specialist, then a second series from an anesthesiologist specializing in pain medicine. Her back pain continued. As her knee became a problem, too, an orthopedic surgeon recommended knee replacement, diagnosing her with osteoarthritis.
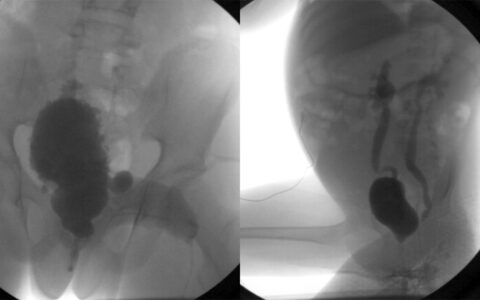
“No studies had been done of her left hip,” Mansourian said. “But during examination, I noticed significant guarding on that side,” he said. “I sent her for X-rays, which showed a fracture in her femoral neck. After a hip replacement surgery, both her back and knee pain resolved.”
“Instead of just accepting radiology reports and proceeding with therapy,” said Mansourian, “it’s important to listen and observe as carefully as possible during every evaluation.”
Rehabilitation Beyond the Acute Phase
A holistic approach includes considering the full roster of treatment options, from physical therapy to diet and medications.
Among Mansourian’s current research and clinical interests: Celiac disease and gluten sensitivity. After seeing the multiple ways celiac disease can present itself in rehabilitation cases – including neuropathy, arthritic pain or osteoporosis, hallucinations or changes of mental state and chronic diarrhea or constipation – Mansourian recommends physiatrists consider a celiac panel, vitamin D or B12 level check as one component of patient assessment.