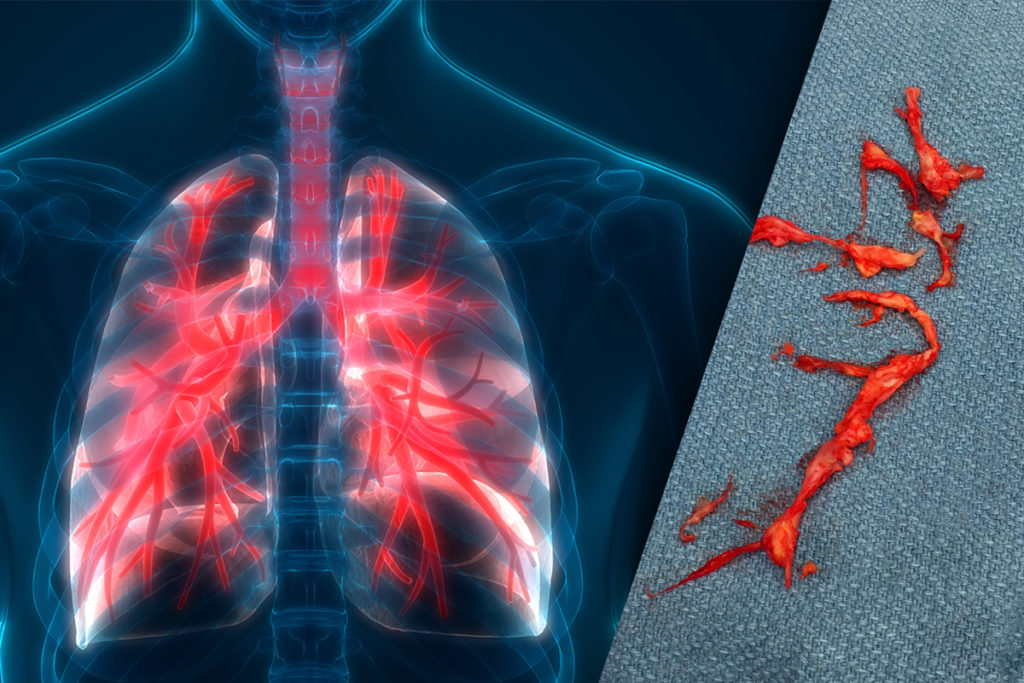
Chronic thromboembolic pulmonary hypertension (CTEPH) can develop in patients who have experienced an acute pulmonary embolism (PE). In CTEPH, it is believed that scar tissue from the site of the initial PE builds up in the lungs and obstructs the blood vessels, causing shortness of breath and pulmonary hypertension. Patients who present with CTEPH may have severely limited daily capabilities.
About three quarters of patients with CTEPH will give a history of an acute PE, often several years previously. CTEPH is underrecognized; there are approximately 600,000 cases of PE per year in the United States, and as many as 4% of patients can develop the condition.
“Of all the causes of pulmonary embolism, you don’t want to miss this diagnosis since it’s the only form of pulmonary hypertension that has the potential to be cured,” said Ivan Robbins, M.D., director of the Adult Pulmonary Vascular Center at Vanderbilt University Medical Center. “Unfortunately, it often goes undiagnosed. If you suspect a patient has CTEPH, you should send them for further evaluation to a treatment center that specializes in pulmonary vascular disease.”
How Is CTEPH Diagnosed?
Specialized tests and imaging studies to confirm a diagnosis of CTEPH may include:
- Echocardiogram – An echocardiogram alone cannot diagnose CTEPH, but it can determine if the patient has some type of pulmonary hypertension.
- Ventilation-perfusion (V/Q) scan – Radioisotopes are inhaled and injected intravenously to determine if there are areas of the lung where blood circulation is compromised. This is the recommended screening test for CTEPH. A normal result from a V/Q scan means a patient does not have CTEPH.
- Pulmonary angiography – Dye is injected directly into the pulmonary arteries and pictures are taken. There are characteristic findings of CTEPH, and this test is considered the “gold standard” for diagnosing the condition.
- Right heart catheterization with echocardiogram – The extent of impairment is evaluated by right heart catheterization, which checks blood pressure and flow in the pulmonary arteries.
- Computed tomography pulmonary angiogram – A CT scan that shows visual slices of the pulmonary arteries and lung tissue. In some cases, this can be used to diagnose CTEPH.
If testing confirms CTEPH, a pulmonary endarterectomy (PEA) is the best treatment option if the patient is a surgical candidate. PEA is a surgical procedure that removes obstructive thromboembolic material from the pulmonary arteries. It can relieve pulmonary hypertension, reduce pulmonary vascular resistance and improve right ventricular function. Despite the need for careful pre-operative assessment, it is important not to delay surgery in eligible patients.
“When a patient has CTEPH,” explained Michael Petracek, M.D., clinical professor of cardiac surgery at VUMC, “surgery is really the only option. Pulmonary endarterectomy offers excellent outcomes – greater than 95% survival rate – and is potentially curative.”
Which Patients Are Candidates for PEA?
The best candidate for PEA is younger than 65 with good organ function. But there is really no age cutoff; patients aged 65 or older without other significant comorbid illness may also be good candidates. While recovery time varies depending on the type of disease, the patient must remain anti-coagulated for life and have regular follow-up visits. With careful patient selection, surgical expertise and post-operative management, PEA offers a life-changing option for patients with complex arterial disorders.
Pulmonary Endarterectomy Resources
Currently, only a few surgical centers have performed PEA in significant numbers. Vanderbilt Heart and Vascular Institute is the only center in the Mid-South with this surgical expertise. “This is not a routine procedure,” said Petracek. “In addition to surgical expertise, it involves specially trained anesthesiologists, radiologists, pulmonologists and cardiologists. It’s important to send the patient to a center where pulmonary endarterectomy surgery is performed regularly.”