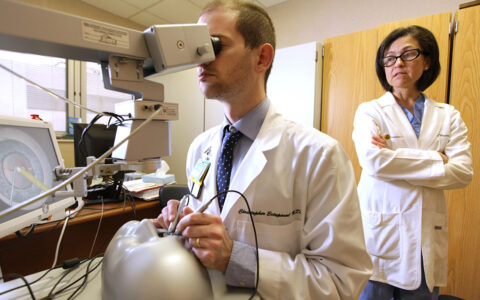
There are fewer than 100 dedicated uveitis specialists in the United States, making access to care challenging for many patients. At the Vanderbilt Eye Institute, Stephen J. Kim, M.D., and Sapna Gangaputra, M.D., provide care to both adults and children with uveitis from across the Southeast, with a special interest in pediatric cases.
Uveitis is one of the most challenging disorders for ophthalmologists to diagnose and treat – especially in children, where it is more likely to cause chronic inflammation and subsequent visual impairment, say the researchers.
The institute’s uveitis service is engaged in multiple research initiatives, including the multicenter, NIH-funded Adalimumab in Juvenile Idiopathic Arthritis-associated Uveitis Trial (ADJUST). Biologics such as adalimumab (marketed as Humira®) have been shown to be effective in treating various subtypes of uveitis, especially in more treatment-resistant cases. The cross-cutting trial requires careful collaboration with pediatric rheumatologists at Vanderbilt and more than 20 other participating institutions.
“We tackle noninfectious chronic uveitis in children by placing patients on systemic immunosuppression early, thereby minimizing their exposure to corticosteroids and their side effects,” said Kim, the Phyllis S. and William B. Snyder Chair and retina division chief in the Department of Ophthalmology and Visual Sciences. “Biologics like adalimumab are very specific; they inhibit a specific signal in the inflammatory cascade and result in better control and better outcomes in many cases.”
“We’re confident adalimumab works; we just don’t know the best time to stop treatment,” said Gangaputra, a uveitis specialist and director for clinical trials at the institute. “The results of ADJUST will provide information to guide clinicians in their decision-making regarding discontinuation.”
Augmenting the Toolbox
Standard local treatments for uveitis include corticosteroid eyedrops, injections or fluocinolone acetonide implants. In another clinical trial, the Vanderbilt researchers will participate in evaluating the safety and tolerability of a nonsteroidal drop for non-infectious anterior uveitis in adults.
“An effective nonsteroid drop will be life-changing for patients who have to use drops daily for the remainder of their lives,” Gangaputra noted.
In addition to new therapeutics, the researchers are interested in the microbiome as it relates to uveitis.
“In children with uveitis, there is some concern as to whether their diets help or hurt their response to treatment,” Gangaputra said. “We need better means of testing.”
Gangaputra has another NIH grant to conduct a retrospective study of uveitis patients who have undergone cataract and glaucoma surgery as a result of the disease. The study will leverage data gathered over a 25-year period on more than 9,000 patients, she said.
Personalized Uveitis Diagnosis
Both researchers note that uveitis presents as a broad spectrum of symptoms, and it is often misdiagnosed.
Some uveitis-related diseases have clinical diagnoses that can be detected on exam and require little lab analysis. In other cases, the patient is diagnosed with an autoimmune disorder by a rheumatologist before they come to the Vanderbilt Eye Institute. Often, the etiology is unknown.
“Because uveitis-related diseases are so heterogeneous, precise diagnosis is critical,” Kim said. “If children don’t receive appropriate intervention as early as possible, they’ll suffer vision loss from structural damage.”
Beyond the standard eye exam, Kim and Gangaputra employ a custom workup including bloodwork, imaging and genetic analyses of intraocular fluid, which can be done in real time in the institute’s laboratory. Given the need for immediate intervention, every child is seen within two weeks of referral.
A major challenge is compliance with follow-up care.
“Because there are so few uveitis specialists, patients must travel long distances for appointments, which can disrupt their lives for a year,” Gangaputra explained. “It’s difficult to explain to people why they need to come back here.”
Educating Trainees and Peers
While uveitis is rare, it is a major cause of blindness, and Gangaputra says it is important to expose residents and fellows to the disease. “We want them to understand the basic infrastructure of uveitis – how to identify it and how to know when you cannot manage it and need to refer to a specialist,” she said.
The same holds true for community physicians. In fall 2021, the Vanderbilt Eye Institute hosted the first Carolyn Smith Uveitis Symposium, with expert presenters from institutions across the U.S. The virtual symposium attracted 170 attendees worldwide. Gangaputra is planning the next symposium and hopes to make it an annual event.